Understanding the cell waste disposal problems in Lou Gehrig’s disease
Building up cellular waste is bad news for cells, and particularly for neurons. Such excessive build up can lead to neurological conditions, as is the case of amyotrophic lateral sclerosis (ALS), also called Lou Gehrig’s disease. Researchers agree that the build up arises from an imbalance between the synthesis and degradation of proteins within cells that leads to progressive, fatal neuronal and muscular degeneration. How this happens, however, is not well understood, but research at Dr. Hugo Bellen’s lab has revealed a novel key connection between ubiquilins and a ‘waste disposal and recycling center’ of the cells.
“Mutations in UBQLN2 and UBQLN4, genes that encode ubiquilins, have been linked to ALS and frontotemporal dementia, a condition similar to Alzheimer’s disease. Although ubiquilins are known to play crucial roles in various biological processes, there was no clear mechanistic understanding of how ubiquilin loss led to progressive neurodegeneration,” said corresponding author Dr. Hugo Bellen, professor of molecular and human genetics and neuroscience at Baylor College of Medicine and an investigator at the Howard Hughes Medical Institute.

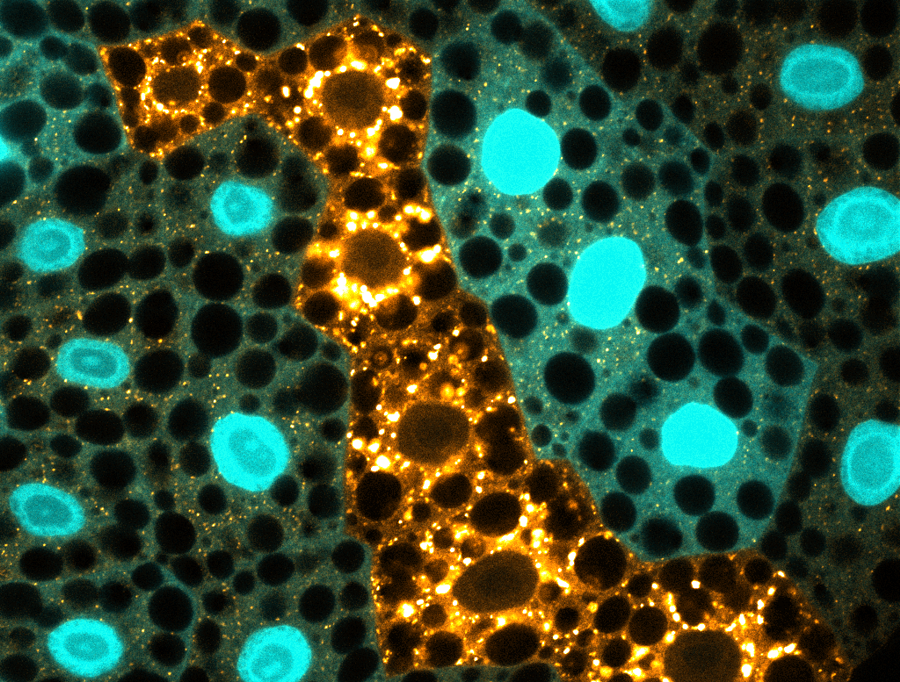
To understand that link, Mümine Şentürk, a graduate student in the Bellen lab and first author of the study, conducted initial experiments in fruit flies lacking the gene ubiquilin. These mutant flies showed signs of progressive age-dependent neurodegeneration, such as impaired neuronal function, death of neurons and increased accumulation of aberrant lysosomes.
Previous studies had shown that ubiquilins are involved in tagging dysfunctional proteins for their disposal in the proteasome. However, defects in the proteasome clearing process alone could not explain the dramatic loss of neurons that the researchers observed in these mutants and suggested that some other pathway was perturbed.
Further studies showed that autophagy, another natural process involved in discarding excess or dysfunctional proteins, also appeared to be defective in ubiquilin mutants.
This suggested that a combined malfunction in the proteasomal and autophagic clearance mechanisms was responsible for the massive build up of dysfunctional proteins and eventual death of these neurons,” said Şentürk.
Autophagy – which means ‘self-eating’ – is a multistep process. First, vesicles called autophagosomes engulf damaged proteins. Then, autophagosomes fuse with lysosomes, vesicles whose acidic environment activates enzymes that degrade cellular waste. So, the researchers next set out to pinpoint which step of autophagy was being affected in the absence of ubiquilin.
“To our surprise, we found that in ubiquilin mutant flies the lysosomes were not acidified, which meant that enzymes that digest cellular garbage could not be activated, leading to waste accumulation,” Şentürk said.

When the researchers fed acidic nanoparticles to the flies to restore the acidic environment inside the lysosomes, clearance of accumulated trash and the normal flow of the process improved.
“Interestingly, we observed the same lysosomal degradation defects in human neuronal cells lacking ubiquilins, suggesting an evolutionarily conserved role for these proteins in regulating the clearance pathways,” said Bellen, who also is a member of the Jan and Dan Duncan Neurological Research Institute at Texas Children’s Hospital. “Further studies are needed to test whether acidic nanoparticles also can promote the survival of neurons in the brains of intact mammals. Nevertheless, we are very excited by the initial success of this strategy in reducing the build up of dysfunctional proteins in flies since it could potentially be developed as a novel therapeutic approach to treat ALS and frontotemporal dementia.”
Go to the journal Nature Cell Biology to read all the details of this study.
Other contributors to this work include Guang Lin, Zhongyuan Zuo, Dongxue Mao, Emma Watson and Antonios G. Mikos. The authors are affiliated with Baylor College of Medicine, Texas Children’s Hospital and Rice University.
Financial support for this project was provided in part by the Baylor College of Medicine Intellectual and Developmental Disabilities Research Center Neurovisualization Core (U54HD083092) from the Eunice Kennedy Shriver National Institute of Child Health & Human Development. Further support was provided by a Ruth L. Kirschstein Fellowship from the National Institute of Dental and Craniofacial Research (F31 DE027586), the Robert A. and Renee E. Belfer Family Foundation, the Huffington Foundation, Target ALS and the NIH Office of the Director (R24OD022005).