Study seeks to identify biological markers that predict mesothelioma response to treatment
The National Cancer Institute (NCI) has granted a $2.5 million, five-year R37 MERIT Award to Dr. Bryan Burt, associate professor of surgery and chief of the Division of General Thoracic Surgery, for his research project titled, “Proteomic Determinants of Response to Checkpoint Blockade in Malignant Pleural Mesothelioma.”

“Malignant pleural mesothelioma (MPM) is a fatal cancer of the lining of the lungs that has defeated standard therapies for decades. In recent years, emerging clinical data has shown that treatment with a form of immunotherapy called immune checkpoint inhibitors (ICIs) results in meaningful extension of life in half of patients with MPM, but is associated with immune-related side effects,” Burt said.
The goal of this study is to develop a clinically relevant test that would enable physicians to determine whether a patient would be most likely or less likely to respond to ICIs before the patient gets treatment, saving those less likely to respond from immune-related adverse events.
We want to be able to predict not only who is going to respond, but also the strength of the response.”
“In other words, whether the tumor will completely or partially shrink or just remain stable for long periods of time, which is important too,” Burt said. “We hope to design a test that would allow us to predict those possible outcomes.”
To develop the test, Burt is taking a closer look inside MPM tissues.
“Preliminary data collected retrospectively showed that the tumors of patients who respond to ICIs tend to have a certain immune cell composition, which is quite complex,” Burt said.
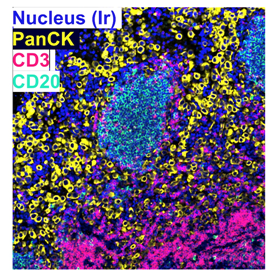
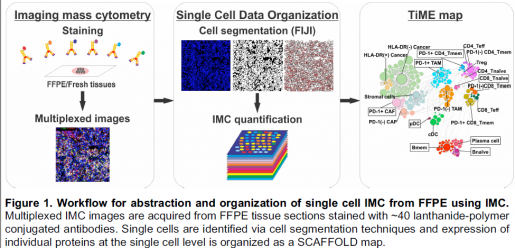
We developed a technique to analyze the presence of about 30 different cell types in a very small bit of a tumor sample.”
Burt also is looking at the architecture of the tissue samples. “In addition to determining how many cells there are of each type, we also study tissue architecture to see how these cells are organized in the tumor. Are they close to blood vessels? Are they close to each other? Our preliminary data showed that tissue immune cell architecture in the tumor also predicts response to treatment,” Burt said.
The study also seeks to better understand the biological mechanism supporting the responders.
“Our preliminary data suggested that MPMs with high levels of neoantigens, new tumor surface molecules that can warn the immune system of the presence of the tumor, is not the only requirement for responding to ICIs,” Burt said. “It’s also important to take into consideration molecules called MHC, which present neoantigens to the immune system and facilitate the stimulation of the soldier immune cells. We have found that when both neoantigens and certain MHC molecules are there, the patient responds well to the therapy.”
Burt hopes that the analyses of tumor neoantigens and HLA molecules can be developed into a test to predict response to ICIs, but also that it will help understand neoantigen biology that could be applicable to other tumors as well.
We anticipate that after this study supported by the R37 MERIT Award we will be able to use both cellular organization and neoantigen:MHC concordance to predict response to ICIs,” Burt said.
“It will then be time for a clinical trial to conduct a rigorous prospective evaluation in which treatment depends on the results of the test.”
Burt’s research submission to the NCI as an R01 application received a score within the NCI pay line for experienced investigators and was thus converted to an R37 MERIT Award. This award enables National Institutes of Health institutes, such as the NCI, to give investigators with stellar records of research accomplishment a five-year award with the possibility of extension for additional years without undergoing another Integrated Review Groups (IRG) peer review. Burt’s five-year award has an opportunity for an extension of up to two additional years. The plan is to conduct the study between 2021 and 2028.