Ebola not the first disease to frighten the public
Those who cannot remember the past are condemned to repeat it. – George Santayana
The current furor over Ebola, a viral infection, and the few cases that have come into the United States or occurred among health care workers brings to mind earlier panics that occurred as diseases happened in the United States. What truly comes to the fore is the courage of health care workers who took or take care of patients, whether their own lives are at risk or not.
Polio
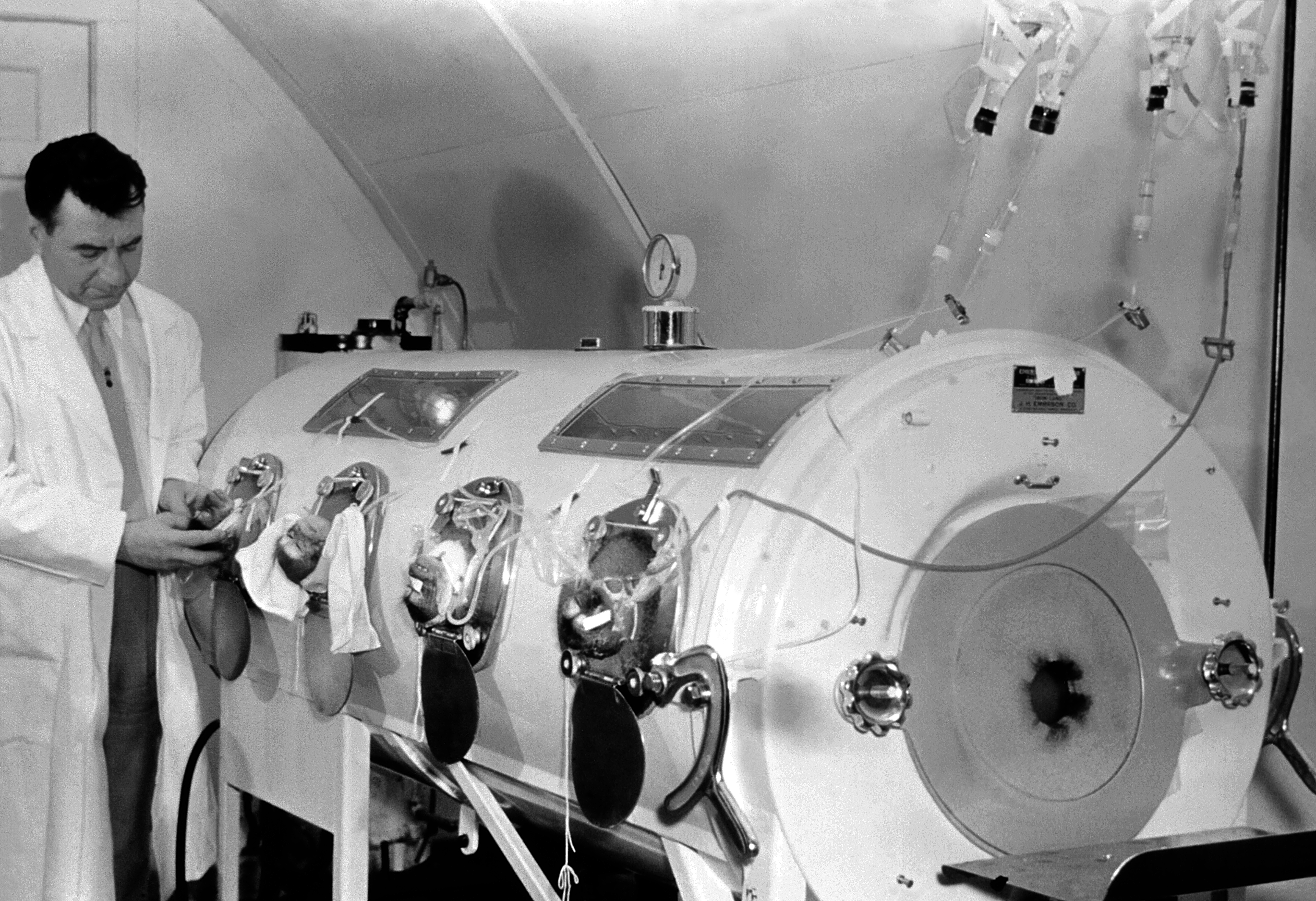
When I was a little girl, parents were terrified that their children would get polio. Public officials closed the swimming pools; children were kept indoors at dusk, when it seemed that the disease was most often to strike. Too often, a child went to sleep seemingly healthy and woke up sick – unable to move limbs and struggling to breathe.
Newspapers were filled with photos of children in iron lungs, and fear filled the air, particularly in the summer when the disease incidence increased. In the early 1940s, When President Franklin Delano Roosevelt, himself a victim of the disease, pushed the establishment of a systematic research program to find what caused polio and the best way to take care of those who had it.
Once a year, my mother and her friends walked from house-to-house, collecting dimes that went to the organization that became the March of Dimes. I will never forget the look on her face when she learned that the clinical trial of a polio vaccine had worked. As soon as it became available, my sister and I received the Salk vaccine. Later, with hundreds of our fellows, we lined up to receive the oral Sabin vaccine as well.
Today, polio has been eradicated for the most part in the industrialized west, but it remains in pockets of poverty – Nigeria, Pakistan, and Afghanistan. As long as one person remains infected with the poliovirus, the risk of getting the disease remains. And we should applaud those workers who continue, often at the risk of their own lives, to get vaccine to children and perhaps eradicate this disease from the Earth.
HIV/AIDS
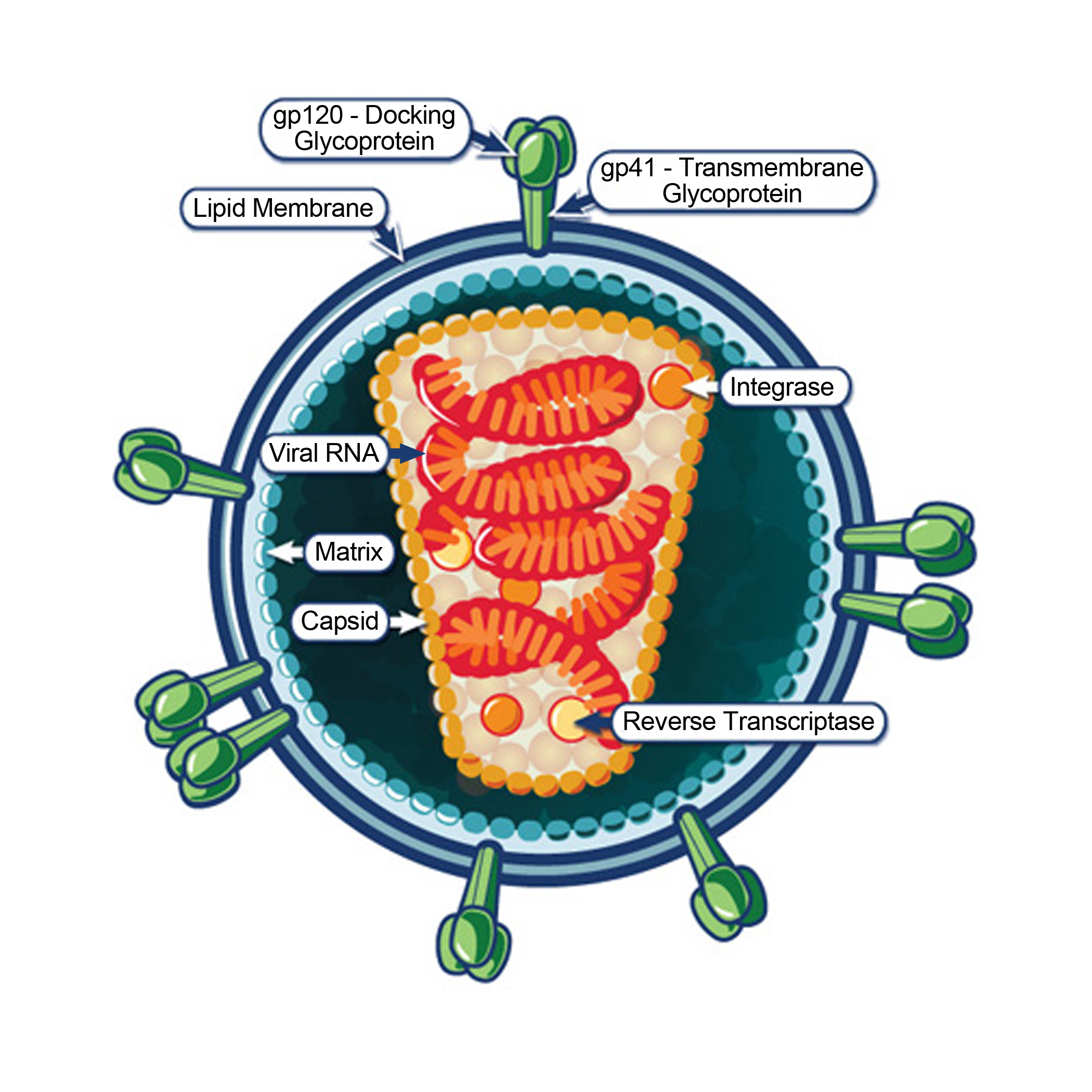
In June 1981, the federal Centers for Disease Control and Prevention published the first report of an odd cluster of cases of cases ofPneumocystis carinii pneumonia in Los Angeles, California. Pneumocystis pneumonia, the experts noted, was limited to severely immunosuppressed patients. Slowly the numbers of patients with this and other so-called opportunistic infections climbed. With it came hysteria. In 1983, the virus that causes AIDS – human immunodeficiency virus or HIV – was discovered, but it did not limit the fear.
During a mayoral campaign in Houston, one of the candidates seemed ready to sign onto a “health card” measure that would require all people who worked in food-service capacity to register and prove they did not have AIDS. Public health experts opposed the measure, and AIDS activists were appalled. In polling the health care population about the response to the measure, I was most taken with the response of one nurse: “We took care of people with polio for years, and we didn’t know what caused that.” To her, the fear was hysteria and politics — not science and health care.
Over the next decade and a half, scientists chipped away at the problem, identifying how the virus worked and how it invaded cells. Then they began to develop drugs that interrupted that process. As the disease became more treatable, people in the United States became less fearful. However, cases of AIDS continue in the Third World and treatment is difficult to obtain in many nations. Stigma continues.
Ebola
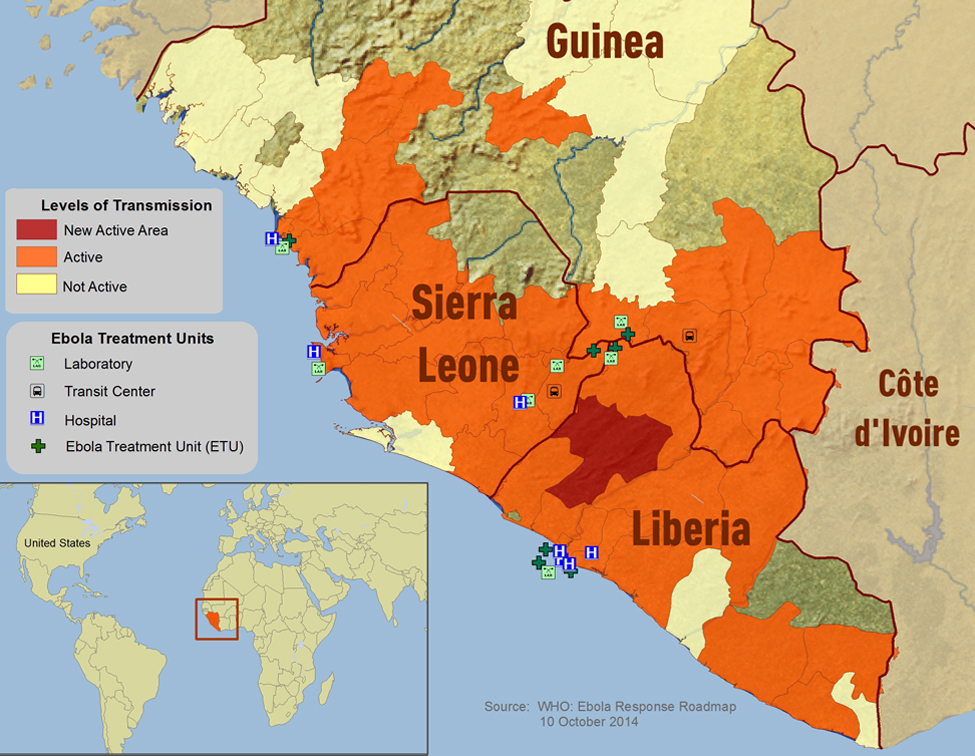
Ebola is not a new disease. It was first recognized in 1976, but until this year, outbreaks were limited to small rural areas of Africa. As it invaded the urban areas of Liberia, Sierra Leone and Guinea, the threat became more obvious. Inevitably, one person infected with the disease who did not know he had it came to the United States and ended up in a Dallas hospital.
The hysteria that accompanied that event resulted in Canada refusing visas to people from countries in with the disease was identified at that time. In the United States, some states instituted quarantine requirements for anyone who had worked with Ebola patients in west Africa, resulting in a furor that affected both New Jersey and Maine.
Not surprisingly, the encroachment of Ebola into the Western Hemisphere pushed the research agenda. Already, a potential vaccine is scheduled for testing. The United States, Canada and other western nations have promised new facilities and equipment that can help treat the disease in those countries where it most prevalent. Across the world, brave health care workers are gathering their equipment and journeying to Africa to join in the fight. They should be applauded for their courage and selflessness.
Perhaps this time, a treatment and a vaccine will come out of tragedy. And it is time that we address the health problems – tuberculosis, malaria and neglected tropical diseases – that afflict the less empowered parts of the world without waiting for a crisis to push us into doing the right thing.
-By Ruth SoRelle, M.P.H. This story originally appeared in the November edition of From the Labs.



