Novel combination therapy offers promising results for treatment-refractory hepatoblastoma
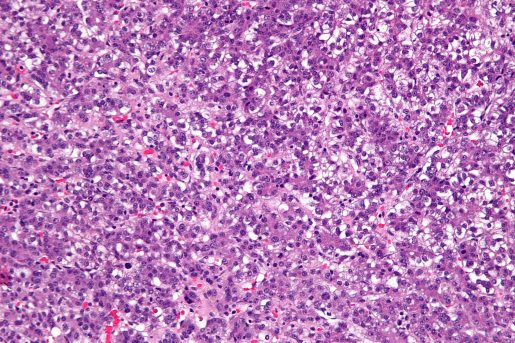
Hepatoblastoma (HB) is the most common liver cancer in children. Researchers and physicians in the field are concerned because in the last decade HB has been rising rapidly worldwide and has seen the most rapid increase among all pediatric solid tumors.
A team led by researchers at Baylor College of Medicine has been working on improving therapies for this devastating disease. They recently reported in the Journal of Hepatology a novel treatment strategy that produced encouraging results in animal models.
“High-risk disease leads to high rates of relapse and mortality,” said first author Dr. Andrés F. Espinoza, general surgery resident in Baylor’s Michael E. DeBakey Department of Surgery.

“In this study, we investigated the potential benefits of a new combination therapy that included an inhibitor of the enzyme histone deacetylase (HDAC) present at elevated levels in HB cells,” Espinoza said. “Previous studies have suggested that HDAC inhibitors may provide treatment options for HB, but there is no published preclinical data on such therapies.”
To assess the effects of the novel combination therapy, the researchers developed a preclinical testing pipeline with clinically relevant HB models.
Identifying an effective new combination therapy
First, the researchers tested several HDAC inhibitors on their ability to kill patient-derived HB cell lines grown in the lab. They found that HDAC inhibitor panobinostat was the most effective at eliminating cancer cells.
The team then tested whether adding panobinostat to current chemotherapy regimens would improve tumor response. They screened these treatments in patient-derived spheroids, spherical cellular aggregates derived from human tumor samples. Their results show that adding panobinostat to the combination treatment including vincristine and irinotecan eliminated more tumor cells than any of the other combinations.
Finally, they tested the new combination therapy of vincristine, irinotecan and panobinostat (VIP) in four aggressive animal models of HB the researchers had derived from high-risk, relapsed and treatment refractory HBs. The molecular characterization of these tumors in the animal models showed that they conserved all mutations found in the human tumors of origin as well as other molecular markers present in patient tumor samples. This indicated that the tumors in the animal models closely matched those in the patients. Importantly, in contrast to other studies that tested treatments on small-sized tumors, this study tested VIP in large tumors.

After just one week of therapy, the tumors that were treated with VIP had a significant decrease in volume and alpha fetoprotein levels, the tumor marker,” said corresponding author Dr. Sanjeev A. Vasudevan, associate professor of surgery at Baylor.
These findings are very encouraging as they suggest that VIP therapy may be a promising and effective option for patients with currently untreatable high-risk, relapsed or refractory HB.”
Other contributors to this work include: Roma H. Patel, Kalyani R. Patel, Andrew A. Badachhape, Richard Whitlock, Rohit K. Srivastava, Saiabhiroop R. Govindu, Ashley Duong, Abhishek Kona, Pavan Kureti, Bryan Armbruster, Dina Kats, Ramakrishnan R. Srinivasan, Lacey E. Dobrolecki, Xinjian Yu, Mohammad J. Najaf Panah, Barry Zorman, Stephen F. Sarabia, Martin Urbicain, Angela Major, Karl-Dimiter Bissig, Charles Keller, Michael T. Lewis, Andras Heczey, Pavel Sumazin, Dolores H. López-Terrada and Sarah E. Woodfield.
The authors are affiliated with Baylor College of Medicine, Texas Children’s Hospital, Children’s Cancer Therapy Development Institute at Beaverton or Duke University.
This work was supported by a U.S. Department of Defense Career Development Award (W81XWH-21-1-0396 /CD201061), a Baylor College of Medicine Michael E. DeBakey Department of Surgery Faculty Research Award, a Macy Easom Cancer Research Foundation Grant, a Cancer Prevention and Research Institute of Texas (CPRIT) Multi-Investigator Research Award (RP180674), a P30 Cancer Center Support Grant NCI-CA125123, a CPRIT Core Facilities Support Grant RP220646 and an NIH Ruth L. Kirschstein National Research Service Award Individual Postdoctoral Fellowship (1F32CA278313-01).
Follow From the Labs on X @BCMFromtheLabs and Instagram!