Eliminating gene SRC-3 in immune cells triggers effective long-lasting anti-cancer response
Researchers at Baylor College of Medicine have discovered a crucial regulator of the anti-cancer immune response that could change the game in the fight against cancer. Published in the Proceedings of the National Academy of Sciences, the study shows that in animal models of breast and prostate cancer, eliminating the gene SRC-3, specifically in a type of immune cell called regulatory T cells (Tregs), triggered a lifelong anti-cancer response that eradicated the tumor without the typical side effects observed with other therapies.
Furthermore, transferring Tregs without SRC-3 to animals carrying breast cancer tumors also resulted in long-term elimination of the tumor without negative side effects. The findings encourage pursuing further investigations to determine the value of this approach to treat the human disease.
Building up on years of research
“More than 30 years ago, my lab discovered a protein we called steroid receptor coactivator (SRC) that is required for the effective regulation of gene activity,” said corresponding author Dr. Bert W. O’Malley, chancellor and professor of molecular and cellular biology at Baylor. “Since then, we have discovered that a family of SRCs (SRC-1, SRC-2 and SR-3), regulates the activity of a variety of cellular functions.”

Over the years, the O’Malley lab and colleagues have been particularly interested in SRC-3 and its role in cancer. SRC-3 is not only highly expressed in all human cancers and plays a role in cancer growth, but it is also strongly expressed in Tregs that regulate the immune response to cancer. Intrigued by the abundance of SRC-3 in Tregs and suspecting that it might play a role in controlling cancer progression, O’Malley and his colleagues investigated the effect of eliminating the gene SRC-3 in Tregs on breast cancer growth.
SRC-3 knock-out Tregs are key to cancer eradication
The team generated mice lacking the SRC-3 gene only in Tregs (SRC-3 knock-outs) and then compared breast cancer progression in these mice with the progression in mice that had the SRC-3 gene.
“We were surprised by the results,” O’Malley said. “Breast tumors were eradicated in the SRC-3 knock-outs. A subsequent injection of additional cancer cells in these mice did not give rise to new tumors, showing that there was no need to generate additional SRC-3 knock-outs to sustain tumor resistance.
Importantly, transferring these cells to animals carrying pre-established breast tumors also resulted in cancer eradication. We obtained similar results with prostate cancer.”
Tregs modify the tumor microenvironment
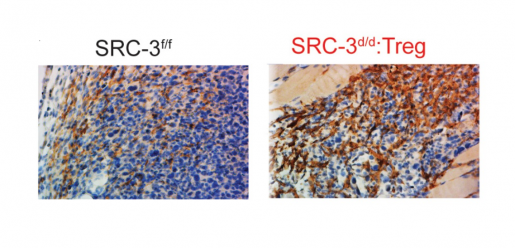
The team also discovered that Tregs lacking SRC-3 mediated long-lasting tumor eradication by effectively modifying the environment surrounding the tumor into one that favored its elimination.
Using a variety of laboratory techniques, O’Malley and his colleagues discovered that the modified Tregs proliferated extensively and preferentially infiltrated breast tumors where they released compounds that generated an anti-tumor immune response. On one side, the compounds facilitated the entrance of immune cells – T cells and natural killer cells – that directly attacked the tumor and, on the other side, modified Tregs blocked other immune cells that attempted to stop the anti-tumor response.

“Other published treatments seem to reduce tumor burden or eliminate the cancer for some time, but in most cases it returns. Our findings in animal models are the first to show that Tregs lacking SRC-3 eradicate established cancer tumors and appear to confer long-lasting protection against recurrence,” said first author Dr. Sang Jun Han, associate professor of molecular and cellular biology and in the Center for Reproductive Medicine at Baylor. He also is a member of Baylor’s Dan L Duncan Comprehensive Cancer Center. “We are very excited about the results; altogether they warrant continuing our investigations to translate the findings into a novel, more effective and longer-lasting cancer therapy.”
Other contributors to this work include senior scientists Dr. David M. Lonard and Dr. Cliff C. Dacso and lab members Prashi Jain, Yosef Gilad, Yan Xia, Nuri Sung, Mi Jin Park, Adam M. Dean, Rainer B. Lanz, Jianming Xu, all at Baylor.
This work is partly supported by funding from the National Institutes of Health grants R01HD07857, R01HD08188 and R01HD098059 and CoRegen, Inc.
Baylor has partnered with CoRegen, Inc. to commercialize these groundbreaking discoveries. All the patents and intellectual property underlying these discoveries have been licensed to CoRegen, Inc.
Follow From the Labs on Twitter @BCMFromtheLabs.