Debunking COVID-19 vaccine misinformation
Two COVID-19 vaccines are now approved for emergency use in the United States, and millions of frontline healthcare workers have started receiving their vaccinations.
But how does the vaccine work? And are there any differences between vaccines?
Dr. Jill Weatherhead, an infectious disease expert at Baylor College of Medicine, debunks some common misinformation, discusses the science behind the vaccine, and shares her personal vaccine experience in the following Q&A.
Q: Are there any notable differences between the Moderna and Pfizer vaccines?
A: The two vaccines that have received FDA Emergency Use Authorization (EUA) are very similar, including how they work (both are mRNA vaccines) and the side effect profile. Some small differences include the duration in between the two required doses (three weeks for Pfizer and four weeks for Moderna) and temperature storage of the vaccines.
Both the Pfizer and Moderna vaccines provide approximately 95% efficacy against the virus after two injections. This efficacy was equal across age, race, ethnicity and the co-morbidities (such as obesity) that were evaluated.
Q: Does the vaccine contain the virus?
A: The vaccines that have received FDA EUA from Pfizer and Moderna are mRNA vaccines. These vaccines do not contain the virus and thus you cannot get the COVID-19 from the vaccine.
Q: How does a mRNA vaccine work?
A: Messenger RNA (mRNA) contain the instructions on how to make the SARS-CoV-2 spike protein or the receptor binding domain of the spike protein. The mRNA is taken up by a cell into the cytoplasm but does not go into the cell nucleus so it will not become incorporated into the genome. The mRNA instructions are translated into a protein, in this case the SARS-CoV-2 spike protein, using the cell machinery that is already present (ribosomes). The protein then goes to the cell membrane and is presented to other immune cells to make an immune response.
Q: Should I be concerned about potential side effects?
A: Prior to any vaccination it is important to know what side effects to expect as all vaccines can cause side effects. The mRNA vaccines commonly cause local injection site pain (similar to tetanus vaccine). Systemic symptoms more commonly occur in people less than 55 years old and after the second vaccination. These symptoms include fever, fatigue and headache. Signing up for V-safe, a CDC tele-communicating safety monitoring system, allows for further evaluation of vaccine side effects.
Q: Should those who have recovered from COVID-19 still get vaccinated?
A: Because the immune response from natural infection can be varied and it remains unknown for how long natural infection leads to immunity, the CDC and ACIP (Advisory Committee on Immunization Practices) recommend that people who have had COVID-19 receive the vaccine as well.
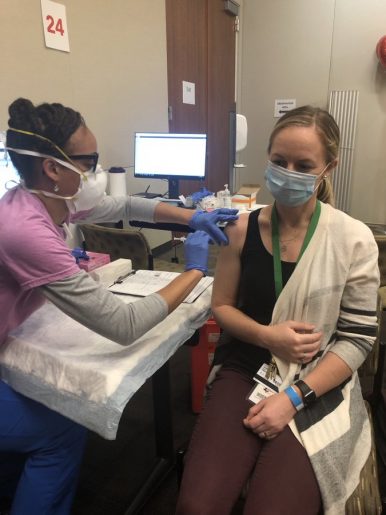
Q: You recently received the vaccine. What was the experience like for you?
A: The experience was very smooth. There was information provided to me before my vaccination, so I felt comfortable about the vaccine and the expected side effects. There were several vaccinators at Texas Children’s Hospital, so it took less than five minutes. I then went to the 30-minute observation area to ensure no adverse events. It was such a positive and hopeful experience.
Q: What would you say to someone who may be reluctant to get vaccinated for various reasons?
A: The vaccines that have so far received FDA EUA approval have been widely tested for both safety and efficacy. The data has been reviewed by independent reviewers to ensure safety. While it seems like these vaccines were made quickly, we must remember that this technology of mRNA vaccines has been in development for years and has been well studied by scientists around the world.
These vaccines are safe. This is a tool that we now have to control this pandemic. If people receive the vaccine when it is their turn, we have an opportunity to control the COVID-19 pandemic faster, with fewer causalities and less long-term health problems.
Dr. Weatherhead is an assistant professor of tropical medicine and infectious diseases at Baylor. See more resources and learn more about the COVID-19 vaccine.
Additional Resources
The COVID-19 vaccine: What you need to know
Tips to stay protected against flu and COVID-19
-By Nicole Blanton



