Common myths and truths about lymphedema
While the true cause of lymphedema is still under investigation, we know that dysfunction in the lymph system results in the collection of lymphatic fluid in one or more areas of the body. We know that patients who have had their lymph nodes removed due to cancer, received chemotherapy, or underwent radiation treatment are more likely to develop secondary lymphedema.

Pre-surgical appointments with your breast and plastic surgeons are incredibly important but can also be overwhelming. Prior to cancer surgery, the focus of the conversation is often centered on your cancer care and reconstruction goals and plan.
However, given the amount of information that those visits need to cover, often the risks and signs of lymphedema after lymph node removal ends up being a secondary concern.
In recognition of World Lymphedema Day on March 6, here are some common myths and truths about this condition.
Myth: I only had a sentinel lymph node biopsy, not an axillary node dissection. I will not get lymphedema.
Truth: The rate of developing lymphedema after axillary lymph node dissection is reported at approximately 20-30%. While the risk of developing lymphedema is indeed much lower amongst sentinel lymph node biopsy patients, it is not zero —the incidence is around 5%. Components of adjuvant cancer treatment such as chemotherapy and radiation are known risk factors for developing lymphedema.
Myth: Flying in an airplane after lymph node surgery will cause lymphedema.
Truth: The only lifestyle-related risk factors for developing lymphedema that have been identified in the literature are weight gain and infections. There is no connection between air travel and lymphedema.
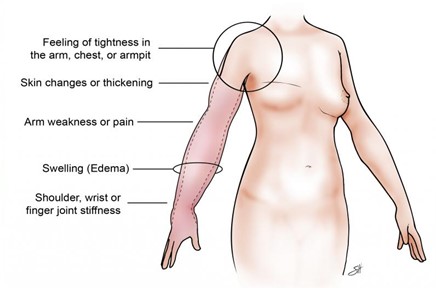
Credit: Scott Holmes
Myth: Vigorous exercise will cause lymphedema and should be avoided.
Truth: This older recommendation has been largely disproven in the literature, and the National Cancer Institute now recommends that carefully controlled exercise is safe for patients with lymphedema. In fact, maintaining normal body weight and avoiding weight gain with supervised exercise and a healthy diet can be beneficial in preventing lymphedema in at risk patients.
Myth: Getting my blood drawn, having my blood pressure taken, or wearing jewelry on the side where lymph nodes were removed will cause lymphedema.
Truth: The recommendations to avoid venipuncture or compression to the limb are old and pervasive but not supported with good scientific evidence. Blood draws and blood pressure readings are safe, although patients may prefer to use the unaffected arm.
When reasonably possible, the goal is to avoid unnecessary trauma or stress to the side where lymph node surgery was performed. We want to avoid skin infection (cellulitis) on the affected arm. Repeated episodes of infection on the affected arm may cause increased damage to the lymphatic system and increase fibrosis.
Myth: Compression garments will not stop my lymphedema from getting worse.
Truth: Compression garments are a key part of the treatment for lymphedema, and in patients with mild lymphedema, they are our first line treatment. In fact, well-fitted compression garments that are replaced after three to six months of continuous use can reliably prevent the progression of lymphedema.
Diligence in wearing compression garments can stabilize and even reduce limb measurements, improve symptoms, and optimize a person’s candidacy for surgical treatments and maximize their benefit after lymphedema surgery.
Myth: I have lymphedema now, and there’s nothing that can be done.
Truth: In addition to compression therapy and limb volume reduction treatments with lymphedema therapists, there are now surgical options for lymphedema. Surgeries include liposuction, microsurgical vascularized lymph node transfer, and lymphovenous bypass using supermicrosurgery. These surgical interventions can both improve your symptoms and also decrease your risk of life-threatening infections.
Additional Resources
Read more about lymphedema surgery services at Baylor Medicine or call 713–798–4321.
Learn more about World Lymphedema Day.
-By Dr. Jessie Z. Yu, assistant professor of surgery in the Division of Adult Plastic Surgery at Baylor College of Medicine



I have lymph node problems on left thigh side grown area. I had one removed in a week another one should up. I been tested for metal allergies etc. bloodwork seems good, so they say, but it has been swollen in upper thigh at least an inch in fluid difference from left to right thigh measurements. left leg will swell up so bad looks like impingement syndrome. i can tell on a normal day left side stays swollen lymph node hurts bad at times. i have two left knee replacements both seems to have failed second one on bone should infection but blood work etc. showed negative but two years its stays swollen. I don’t know what to do or how to resolve this getting tired of people just disregarding it. I am ready to take lower leg off if I can’t find a solution to this problem. i got a total knee replacement and lower back fusion had lymph node ever since…. please advise thank you for your help
I want to know if u can have a robotic knee surgery if u have Lymphodema ? I have it in both legs I do treatments for it I do have swelling and it is never completely gone. If you stand to much it swells. No huge swelling.. if ot what can be done for my severe knee pain?