Tackling the root cause of treatment resistance in age-related macular degeneration
The leading cause of irreversible blindness in the elderly is an aggressive form of age-related macular degeneration known as choroidal neovascularization (CNV). The projected number of people with age-related macular degeneration is 196 million in 2020 and 288 million in 2040.
Anti-vascular endothelial growth factor (anti-VEGF) has revolutionized the treatment for CNV; however, up to one-fourth of all treated patients are unresponsive to this treatment and about one-third of the responders become resistant to it after repeated administration over time.
In his lab at Baylor College of Medicine, Dr. Yingbin Fu, associate professor and Sarah Campbell Blaffer Endowed Chair of Ophthalmology, has been investigating ways to overcome resistance to the promising anti-VEGF treatment, but the journey has been challenging.

“Developing strategies to overcome the resistance has been limited by a poor understanding of its mechanism and the absence of suitable animal models,” Fu said. “Researchers have explored various combination therapies in clinical trials. For example, targeting PDGF (Fovista) or the angiopoietin pathway. However, we still have not found a major breakthrough. In fact, a phase III trial combining anti-VEGF and PDGF failed to demonstrate improved efficacy.”
A new approach to combat anti-VEGF resistance
Fu joined forces with Dr. Longhou Fang, associate professor of cardiovascular sciences at Houston Methodist DeBakey Heart and Vascular Center.

The inspiration for their study came from previous work suggesting that macrophages may play a role in anti-VEGF resistance and that increased cholesterol accumulation in macrophages may promote CNV. Such cholesterol accumulation also has been associated with the formation of abnormal new blood vessels invading the retina, typical of CNV. These vessels leak, which promotes inflammation and rapid damage to photoreceptor (light-detecting) cells.
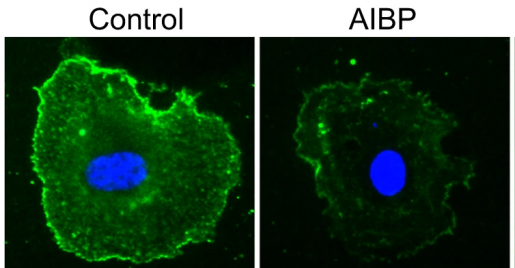
In addition, Fu, Fang and their colleagues, as well as other researchers, had reported that AIBP promotes the removal of cholesterol from endothelial cells and macrophages, two cell types that are involved in the development of CNV.
“Together, these observations suggested the possibility that AIBP might help overcome anti-VEGF resistance and effectively suppress CNV,” Fu said.
Developing an animal model to assess new approach to overcome anti-VEGF resistance
To test their hypothesis, the researchers developed a model of anti-VEGF resistance by combining advanced age with laser delivery in mice. As they became older, the mice showed increased resistance to anti-VEGF treatment that correlated with increased intracellular cholesterol accumulation in macrophages. The researchers tested the effect of AIBP and anti-VEGF in disease progression in this mouse model.
In young mice that were about eight weeks old, both AIBP and anti-VEGF were equally effective in controlling disease progression. In intermediate age mice, which were about eight months old or the equivalent of middle-aged people, macrophages showed increased cholesterol accumulation. In this group, anti-VEGF treatment was less effective when compared with younger mice, but the AIBP treatment was as affective controlling the disease.
The oldest group of mice, which was about 18 months old or the equivalent of senior people, showed highest cholesterol accumulation inside macrophages and were resistant to anti-VEGF treatment. Interestingly, AIBP alone also did not inhibit CNV, but the combination of AIBP with anti-VEGF overcame the anti-VEGF resistance and robustly suppressed laser-induced CNV by 47 percent.
This study also has increased our understanding of the mechanism underlying anti-VEGF resistance. The researchers provide strong evidence that the accumulation of cholesterol in old macrophages plays a central role in anti-VEGF resistance because the old mice became responsive to anti-VEGF treatment when macrophages were chemically depleted. Fu, Fang and colleagues propose that the beneficial effect of AIBP is likely due to both its ability to enhance cholesterol removal from macrophages and its anti-inflammatory function.
Clinical implications
“Our findings encourage us to test the combination therapy of AIBP and anti-VEGF in clinical trials to determine whether it can help patients with the condition,” Fu said. “The projected number of people with age-related macular degeneration is 196 million in 2020 and 288 million in 2040. There is great interest in novel therapies for this devastating condition.”

Co-author Dr. James Handa, Chief of the Retina Division at the Wilmer Eye Institute, Johns Hopkins School of Medicine said, “Age-related macular degeneration has multiple factors that contribute to its development; therefore, future treatments that target multiple pathways, such as what we describe here, may lead to more effective outcomes.”
“As a cardiovascular scientist, my research is centered on cholesterol metabolism and angiogenesis, the formation of new blood vessels. My team has been collaborating with Dr. Fu for several years in developing AIBP as a potential treatment for age-related macular degeneration,” Fang said. “Our studies show that AIBP can be a promising therapy for the treatment of CNV. Compared to the standard anti-VEGF therapy, AIBP targets multiple causes of age-related macular degeneration by correcting the adverse profiles associated with aging. The discovery that the combination therapy can overcome anti-VEGF resistance shows the power of multidisciplinary research.”
Read all the details of this study in the journal Communications Biology.
Other contributors to this work include Lingping Zhu, Mackenzie Parker, Nduka Enemchukwu, Megan Shen, Guogang Zhang, and Qing Yan. The authors are affiliated with one or more of the following institutions: Baylor College of Medicine; Houston Methodist DeBakey Heart and Vascular Center; Xiangya Hospital of Central South University, Hunan, China; Rice University; Johns Hopkins School of Medicine and Weill Cornell Medical College, New York.
This work was supported by grants from BrightFocus Foundation, Retina Research Foundation, the Sarah Campbell Blaffer Endowment in Ophthalmology, NIH core grant 2P30EY002520 to Baylor College of Medicine and an unrestricted grant to Baylor’s Department of Ophthalmology from Research to Prevent Blindness.