The single cell and the cluster, what makes one better than the other at cancer metastasis?
Cancer metastasis is all about rogue cancer cells abandoning the original tumor and venturing through the blood in search for new breeding grounds. Sometimes, single cells take the risk, but other times cancer cells detach from the tumor as clusters.
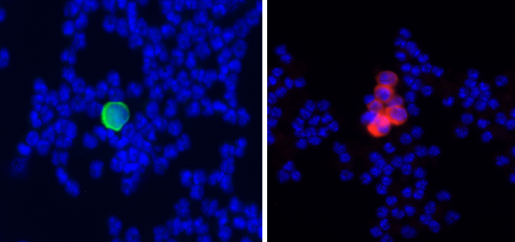
Scientific evidence shows that clusters seem to be more successful at metastasis than single cells and recent work from the laboratory of Dr. Xiang Zhang sheds new light into what contributes to the clusters’ enhanced metastatic abilities.
“We were working with different animal models investigating why tumor clusters seemed to be better at forming lung metastases than single cells, when we unexpectedly discovered that the clusters’ ability to metastasize appeared to be associated with the presence of competent natural killer (NK) cells,” said first author Hin Ching Flora Lo, graduate student in Baylor’s Integrative Molecular and Biomedical Sciences Graduate Program in the Zhang lab. Zhang is professor of molecular and cellular biology and the Lester and Sue Smith Breast Center at Baylor.

The researchers determined that activated NK cells, immune cells that specialize in surveillance and destruction of tumor cells, can eliminate both single cell and cluster metastasis, but they are more efficient at eliminating the former. The clusters have a selective advantage and, as a result, their contribution to metastasis is higher than that of single cancer cells.
“We also explored what mediated the clusters’ resistance to NK cell killing and discovered that cancer clusters seem to tone down the activity of NK cells against them,” Lo said. “Clusters display on the cell surface more molecules that inhibit the activity of NK cells and fewer that increase their activity. As a result, when NK cells bind to clusters to destroy them, the combined effect is reduced killing activity.”

This phenomenon may represent an additional survival advantage complementary to other previously known characteristics of cancer clusters, such as being resistant to chemotherapy.
“Our study highlights the importance of NK cells in immunotherapy. Activated NK cells act fast, and efficiently kill tumor cells. They use a killing mechanism that is similar to the one T cells use, but recognition of the tumor cells is different,” said Zhang, a member of Baylor’s Dan L Duncan Comprehensive Cancer Center and a McNair Scholar.
That’s one of the reasons we think that enhancing NK-mediated killing ability may provide a complementary approach in immunotherapy,” Zhang said.
Interested in reading all the details of this study? Find it in the journal Nature Cancer.
Other contributors to this work include Zhan Xu, Ik Sun Kim, Bradley Pingel, Sergio Aguirre, Srikanth Kodali, Jun Liu, Weijie Zhang, Aaron M. Muscarella, Sarah M. Hein, Alexander S. Krupnick, Joel R. Neilson, Silke Paust, Jeffrey M. Rosen and Hai Wang. The authors are affiliated with Baylor College of Medicine, Courier Therapeutics, Texas Medical Center, University of Virginia, The Scripps Research Institute and the McNair Medical Institute.
This study was supported by the Breast Cancer Research Foundation, National Cancer Institute grants (CA227904, NCI CA148761, NCI CA190467), U.S. Department of Defense (DAMD W81XWH-16-1-0073 and W81XWH-18-1-0574) and the McNair Medical Institute. Further support was provided by CPRIT RP170172, CPRIT Core Facility Support Award (CPRIT-RP180672), The Samuel Waxman Cancer Research Foundation and NIH grants (P01 AI116501, R01 AI145108-01, IO1 IBX0104588A, R41 CA224520-01A1, P30 CA125123, S10 RR024574 and 1S10OD016167).



