AKAP8 and the delicate balance between normal and metastatic states
A protein naturally produced in the body has been found to suppress breast cancer metastasis in animal models of human tumors.
“Our laboratory investigates cellular mechanisms that regulate breast cancer metastasis. In a previous study we provided the first evidence that alternative splicing, a cellular process that enables cells to switch between different forms of the same protein, can functionally control tumor metastasis,” said corresponding author Dr. Chonghui Cheng, associate professor at the Lester and Sue Smith Breast Center, of molecular and human genetics and of molecular and cellular biology at Baylor.

Alternative splicing is a natural cellular process that helps cells conduct many functions, such as wound healing and embryonic development. Through alternative splicing, cells can make a large number of proteins from a limited number of genes. It would be like putting together a number of different outfits by combining in different ways a limited number of pieces of clothing. In humans, around 95 percent of all genes are processed through alternative splicing. Just recently has this process also been shown to be involved in cancer.
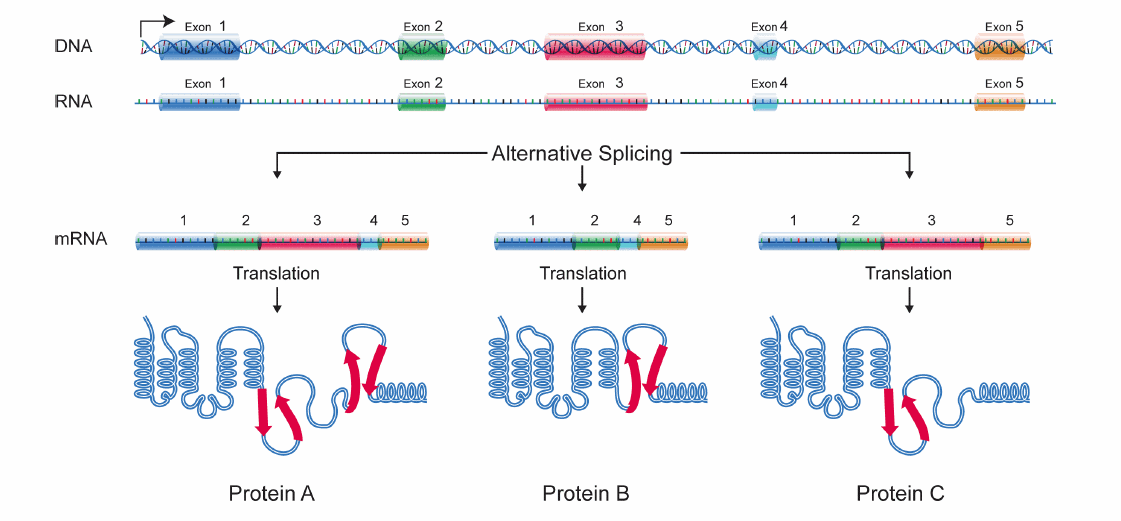
In that pioneering study that brought alternative splicing to the field of cancer research, Cheng and her colleagues showed that of the two distinct forms of the protein CD44 that can be produced by alternative splicing, named CD44s and CD44v, only the former contributed to cancer cell survival. These findings have been confirmed by other reports about breast cancer and also other types of cancer.
In the current study, the researchers further investigated how alternative splicing contributes to cancer metastasis by looking for proteins that regulate alternative splicing events linked to metastasis.
AKAP8 helps keep cells in a non-metastatic state
Cheng and her colleagues screened cells looking for proteins functioning as alternative splicing modulators that prevented cells from becoming metastatic. They identified a set of proteins that were potentially key for tumor metastasis regulation and focused on AKAP8.
“We studied AKAP8 in metastatic breast cancer animal model systems of cancer cells from human patients,” Cheng said. “We found that depletion of the AKAP8 protein in patient cancer cells promoted breast cancer metastasis in these mouse models. Furthermore, providing an external source of AKAP8 inhibited metastasis.”
Taking it all together, the results support AKAP8 as an important regulator of alternative splicing events linked to tumor metastasis. It is not only able to predict metastatic breast cancer outcomes in patients, but also can inhibit metastatic breast cancer progression in animal models.
Cheng and her colleagues continued their investigations to determine how AKAP8 mediated its metastasis-suppressing effects. They discovered that, in addition to modulating alternative splicing of CD44, AKAP8 also regulated the alternative splicing of another protein called CLSTN1. In this case, of the two forms of CLSTN1, named CLSTN1S and CLSTN1L, AKAP8 tipped the balance toward the production of the former, which was associated with preventing cells from progressing toward a metastatic state. This was a previously unknown function of CLSTN1.
“We think that modulators of alternative splicing participate in a delicate balancing act of many different cellular proteins, such as CD44 and CLSTN1. Two types of modulators play a part in keeping the balance. One type, like AKAP8, modulates alternative splicing toward the production of proteins that help cells remain in a normal state. The other type tips the balance toward proteins that promote metastatic transformation,” Cheng said. “If the balance is disturbed, tumor progression can be promoted. By investigating how the balance is kept and the factors that disturb the balance, we hope to understand a new layer of regulation of tumor metastasis and gain insights that could lead to treatments for metastatic cancer, a deadly disease.”
The study appeared in Nature Communications.
Other contributors to this work include Xiaohui Hu, Samuel E. Harvey, Rong Zheng, Jingyi Lyu, Caitlin L. Grzeskowiak and Kenneth L. Scott at Baylor; and Emily Powell and Helen Piwnica-Worms at The University of Texas MD Anderson Cancer Center, Houston.
This research was supported in part by grants from the US National Institutes of Health (5F30CA196118, R01 CA182467, R01GM110146 and R35GM131876) and CPRIT Scholar in Cancer Research grant RR160009.


