Restoring protein imbalance improves memory deficits in Down syndrome
Down syndrome is the most common genetic cause of intellectual disability. The disorder occurs when a person has three, instead of two, copies of chromosome 21. Currently, there is no effective treatment for this condition.
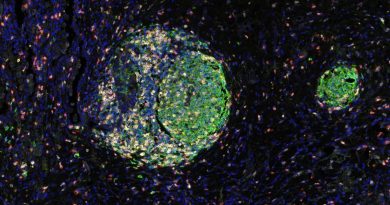
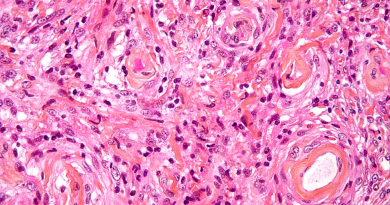
Memory deficits are a hallmark of Down syndrome, but little is known about the mechanisms that lead to them. In his lab at Baylor College of Medicine, Dr. Mauro Costa-Mattioli and his colleagues study at the cellular level mechanisms that are disrupted in Down syndrome looking to identify those that may be involved in causing the condition.

“In the current study, we investigated the role protein homeostasis networks play in Down syndrome. Protein homeostasis networks refers to the cell’s processes geared at maintaining a balance between how much protein is produced and how much is degraded, which is important for keeping cells working properly,” said Costa-Mattioli, professor of neuroscience and Cullen Foundation Endowed Chair at Baylor College of Medicine. “A decline in protein homeostasis networks is strongly linked to several neurological conditions, from aging to neurodegenerative disorders, but little was known about its role in Down syndrome.”
The researchers first discovered that the rates of protein synthesis were reduced in the brains of mouse models of Down syndrome and in human cells isolated from individuals with the condition. But, what was leading to deficits in protein synthesis?
Involving the ‘integrated stress response’
Costa-Mattioli and his colleagues discovered that activation of the ‘integrated stress response,’ or ISR, a network that regulates protein homeostasis by regulating protein synthesis, could explain the protein synthesis deficits associated with Down syndrome.
Motivated by these encouraging findings, the researchers next investigated whether the activation of the ISR mediated the long-term memory deficits in Down syndrome mice. To answer this question, they used four independent genetic and pharmacological manipulations to correct the ISR in a Down syndrome mouse model.
“Down syndrome mice exhibit problems with long-term memory,” said first author Dr. Ping Jun Zhu, assistant professor of neuroscience and senior investigator in the Costa-Mattioli group. “In one set of experiments we trained Down syndrome and control mice in a new task. Down syndrome mice did not learn the task as well as control mice. However, when we genetically or pharmacologically inhibited the ISR, the animals were able to learn almost as well as control mice.”
The researchers also measured the strength of the synaptic connections in the Down syndrome mice and found that the connections were not as strong as those in control mice. But inhibiting the ISR in Down syndrome mice was able to reverse the deficits in synaptic function.
At the cellular level, synaptic plasticity — the ability to form neural connections — is believed to be a central mechanism that could explain how memories are formed, therefore these findings support the researchers’ hypothesis that the activation of the ISR network mediates the memory deficits associated with Down syndrome.
“In the last 10 years, we and others have shown the ISR is a molecular switch for normal long-term memory formation.
In this study, we found that the switch is off in Down syndrome. More importantly, turning the switch back on in these mice reverses their memory deficits,” Costa-Mattioli said.
“These very encouraging results suggest that tuning the ISR may emerge as a promising avenue to alleviate a wide range of cognitive disorders with a disruption in protein homeostasis.”
Find all the details of this work in the in the journal Science.
Other contributors to this work include Sanjeev Khatiwada, Ya Cui, Lucas C. Reineke, Sean W. Dooling, Jean J. Kim, Wei Li from Baylor College of Medicine and Peter Walter from University of California at San Francisco.
This work was supported by funding from the NIH (R01 NS076708, R01HG007538, R01CA193466, and R01 CA228140), Sammons Enterprises and the Howard Hughes Medical Institute.