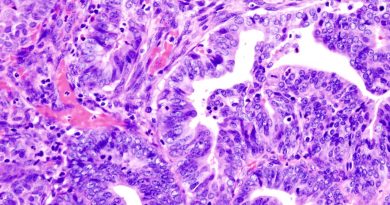
‘Drug factory’ implants eliminate mesothelioma tumors in mice
Rice University and Baylor College of Medicine researchers have shown they can eradicate advanced-stage mesothelioma tumors in mice in just a few days with a treatment combining Rice’s cytokine “drug factory” implants and a checkpoint inhibitor drug.
The researchers administered the drug-producing beads, which are no larger than the head of a pin, next to tumors where they could produce continuous, high doses of interleukin-2 (IL-2), a natural compound that activates white blood cells to fight cancer.

The study, published online today in Clinical Cancer Research, is the latest in a string of successes for the drug-factory technology invented in the lab of Rice bioengineer Omid Veiseh, including Food and Drug Administration (FDA) approval to begin clinical trials of the technology this fall in ovarian cancer patients.
“From the beginning, our objective was to develop a platform therapy that can be used for multiple different types of immune system disorders or different types of cancers,” said Rice graduate student Amanda Nash, who spent several years developing the implant technology with study co-lead author Samira Aghlara-Fotovat, a fellow student in Veiseh’s lab.
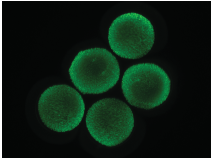
The cytokine factories consist of alginate beads loaded with tens of thousands of cells that are genetically engineered to produce natural IL-2, one of two cytokines the FDA has approved for treatment of cancer. The factories are just 1.5 millimeters wide and can be implanted with minimally invasive surgery to deliver high doses of IL-2 directly to tumors. In the mesothelioma study, the beads were placed beside tumors and inside the thin layer of tissue known as the pleura, which covers the lungs and lines the interior wall of the chest.
“I take care of patients who have malignant pleural mesothelioma,” said Dr. Bryan Burt, professor and chief of Baylor’s Division of Thoracic Surgery in the Michael E. DeBakey Department of Surgery. “This is a very aggressive malignancy of the lining of the lungs. And it’s very hard to treat completely by surgical resection. In other words, there is often residual disease that is left behind. The treatment of this residual disease with local immunotherapy — the local delivery of relatively high doses of immunotherapy to that pleural space — is a very attractive way to treat this disease.”
Veiseh said the mesothelioma study began when Burt and Baylor surgeon and associate professor Dr. Ravi Ghanta heard about the early results of ovarian cancer animal tests Veiseh’s team was conducting with collaborators at the University of Texas MD Anderson Cancer Center. In March, Veiseh and MD Anderson collaborators published a study showing IL-2-producing beads could eradicate advanced-stage ovarian and colorectal tumors in mice in less than a week.
“They were really impressed by the preclinical data we had in ovarian cancer,” Veiseh said of Burt and Ghanta. “And they asked the question, ‘Could we actually leverage the same system for mesothelioma?’”
Mesothelioma refers to any cancer that occurs in the tissue linings that surround and protect internal organs. About 80% of mesothelioma cases are linked to prolonged exposure to asbestos.
Immunotherapy with drugs called checkpoint inhibitors has met with some success in treating mesothelioma. Checkpoint inhibitors don’t kill cancer directly but rather by training the immune system to recognize and destroy cancer cells.
In the mesothelioma study, the Rice-Baylor team tested Veiseh’s drug factory implants both by themselves and in combination with a checkpoint inhibitor that targeted the PD-1 protein. They found the drug factory implants eliminated tumors in more than 50% of the treated animals when used by themselves.
Tumors were destroyed completely in all seven mice that were treated with both the drug factory implants and PD-1 checkpoint inhibitor.
“It’s very hard to treat mesothelioma tumors in mice, like it is in human beings,” said Burt, who also is a member of the Dan L. Duncan Comprehensive Cancer Center at Baylor. “And what our data show is that delivery of these immunotherapy particles, regionally, to these mice who have mesothelioma, has very provocative and very effective treatment responses. In fact, I’ve not seen these mesothelioma tumors in mice be eradicated, with such efficacy, as we have in this mouse model.”
Veiseh said the results also suggested that the combination of IL-2-producing implants and anti-PD-1 checkpoint inhibitors could be effective at training “memory T cells” that can reactivate the immune system to fight mesothelioma if it recurs.

“We have a spinout company, Avenge Bio, that recently received clearance from the FDA to treat ovarian cancer patients, and in the next couple of months they expect to begin treating patients with these IL-2 cytokine factories,” Veiseh said.
“The preclinical data reported in our latest manuscript helped justify initiating a second clinical trial for patients suffering from mesothelioma and other lung cancers with pleural metastasis,” Veiseh said. “We have held meetings with the FDA and expect to initiate a second trial for this patient population in the latter half of 2023.”
Bertha Castillio, Aarthi Pugazenthi, Annie Nguyen and Alexander Lu (Rice University), Hyun-Sung Lee and Hee-Jin Jang (Baylor College of Medicine) and Andrea Hernández (UTHealth Houston), also contributed to this work.
In addition to the cancer research, Veiseh and Ghanta have received a grant from the American Heart Association to study the cytokine implants’ potential for healing heart injuries caused by heart attacks.
The research was funded by the Cancer Prevention Research Institute of Texas (RR160047), the National Science Foundation (1842494) and the National Institutes of Health (R01DK120459-01).
Read more at Rice University news site.