A closer look at genetic and cellular alterations involved in COPD
Chronic obstructive pulmonary disease, or COPD, refers to a group of lung diseases that block airflow and make it difficult to breathe. About16 million Americans have this disease, according to the Centers for Disease Control and Prevention. Although there is no cure for COPD, there are treatments available.

There is a need for a better understanding of the factors and processes involved in the disease and at Baylor College of Medicine the lab of Dr. Ivan Rosas, together with researchers at Yale University and other institutions, has taken a step forward in that direction by investigating the complexity and diversity of cellular injury and inflammation in COPD.

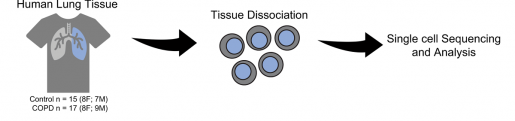
“We used single-cell RNA sequencing to analyze gene expression profiles of lung tissue obtained from patients with COPD and from mice exposed to cigarette smoke,” said Rosas, senior author of the study and section chief of pulmonary, critical care and sleep medicine in the Department of Medicine at Baylor.
The researchers separated all the cells within the lung and measured the gene expression profile of each individual cell. Then, they organized this information in a cell atlas that is available to researchers interested in exploring gene expression in individual cells in lungs with the disease.
“Our analysis identified novel changes in gene expression and cellular interactions in three distinct cell populations commonly implicated in COPD: epithelial (in the lungs), endothelial (in blood vessels) and macrophage cells (part of the immune system),” Rosas said.
The researchers identified a subpopulation of epithelial cells in lungs with COPD that has abnormal expression of genes involved in metabolic, antioxidant and cellular stress responses, when compared to controls.
“In the current study, Drs. Maor Sauler and John McDonough of Yale University, corresponding authors of the work, demonstrate that endothelial cells in capillary blood vessels in COPD lungs are inflamed, and that a subpopulation of macrophages expressing high levels of metallothioneins, proteins that regulate the balance of certain metals in the body, seems to contribute to the disease,” Rosas said.
This innovative translational study is a continuation of a successful long-standing collaboration with Dr. Naftali Kaminski and colleagues at Yale University, which has led to the description of multiple lung cell atlases in health and disease that are now publicly available.
Future studies evaluating outcomes of specific alterations identified in this study will provide further insights into mechanisms that contribute to COPD and having a large and accessible data set of COPD cells, such as the cell atlas here, is an essential tool to begin developing therapies to target the condition.
The research team continues to focus on developing innovative genomic datasets to better understand the pathologic underpinnings of chronic lung disease. They are currently in the process of completing the largest COVID-19 lung fibrosis cell atlas.
Read the complete report in the journal Nature Communications.
For the complete list of authors, their affiliations and financial support for this project see the publication.