Waking up sleeping beauty – persistent IFN-gamma awakens and activates stem cells via BST2
Fighting an infection unleashes a whirl of immunological activity set on eliminating the microscopic invaders. One of the fighters is an inflammatory molecule called IFNγ. Although highly effective, IFNγ has undesirable consequences when persistently produced – it irreversibly exhausts blood stem cells, the progenitors of all blood cells, including immune cells, by triggering their proliferation and excessive terminal differentiation. Lacking immune cells, patients eventually are unable to fight infections.
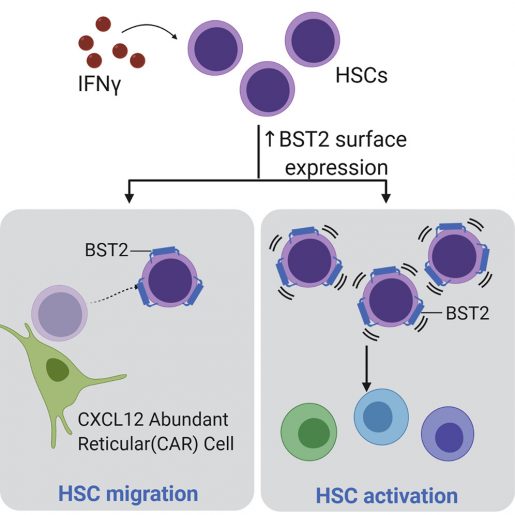
At Baylor College of Medicine, the laboratory of Dr. Katherine King and her colleagues investigated the mechanism by which IFNγ mediates depletion of blood stem cells, which are normally quiescent, meaning they are in a dormant state until activated when stimulated. The researchers hoped that understanding how too much of IFNγ can knock down immune defenses would lead to a solution.
A closer look at stem cells

“We began our investigation by asking, ‘What is changing about blood stem cells when they interact with IFNγ, and how does that influence their reproduction or depletion?’” said King, associate professor of pediatrics-infectious diseases and member of the Dan L Duncan Comprehensive Cancer Center at Baylor.
Blood stem cells reside in the bone marrow, normally in contact with CAR cells that form a sort of a nest. CAR are nurse cells that support stem cell health.
“To investigate the real-time interaction of blood stem cells and CAR cells in live animals, we developed new mouse models designed to express different fluorescent proteins in blood stem cells (red) and CAR cells (green) in the same animals. This model enabled us to visualize and track both cell types individually and simultaneously within intact bones of living animals,” said co-corresponding author Dr. Dongsu Park, assistant professor of molecular and human genetics and pathology and immunology at Baylor.

Combining this approach with advanced live-animal imaging technology, the team discovered a tight interaction between blood stem cells and CAR cells in normal bone marrow, but when exposed to IFNγ, stem cells unexpectedly moved away from CAR cells.
“We think IFNγ is disrupting the quiescent state of stem cells and promoting cell activity,” King said.
“Our next experiments looked at how that was happening.”
The researchers looked for proteins on the surface of stem cells that were expressed after exposure to IFNγ. They hypothesized that probably a surface protein induced by IFNγ was promoting the separation of stem cells from CAR cells.
Think of it as a sticky tag that is on the outside of the stem cells that is pulling them to some other place. That’s how we identified this protein called BST2,” King said.
“In fact, in mice in which we knocked out BST2, the relocalization of stem cells away from the nest and their excessive proliferation and exhaustion did not happen, supporting the role of BST2 in these functions. The findings suggest that modulating BST2 expression on blood stem cells may provide a means to regulate these cells’ activation and/or persistence during chronic infections.”
Homing
The researchers also found that BST2 helps cells bind to E-selectin, a protein on the surface of endothelial cells, such as those lining blood vessels. These findings are relevant to homing, a process by which blood stem cells from a bone marrow transplant find their way to their home in the recipient’s bone marrow.
Homing of stem cells improved when we exposed them to IFNγ. We propose that having more BST2 may help stem cells stick to E-selectin on endothelial cells, facilitating crossing through blood vessels to reach the bone marrow,” King said.

“BST2 is a fascinating protein that has been mostly studied for its ability to both protect our body from viral infections and its role in cancer. I am most excited that we are the first group to report that BST2 plays an important role in blood stem cells, which are at the top of immune system hierarchy,” said first author Marcus A. Florez, a student in Baylor’s Medical Scientist Training Program (M.D./Ph.D.) in the King lab. “This project has important implications in a wide variety of diseases including chronic infections, bone marrow failure and transplant recipients.”
Find all the details of this work in the journal Cell Reports.
Other contributors to this work include Katie Matatall, Youngjae Jeong, Laura Ortinau, Paul Shafer and Anne Lynch at Baylor, and Roman Jaksik and Marek Kimmel at Silesian University of Technology, Poland and Rice University.
Find the complete list of financial support for this project on the publication.