Exceptional responders reveal cancer’s Achilles heel
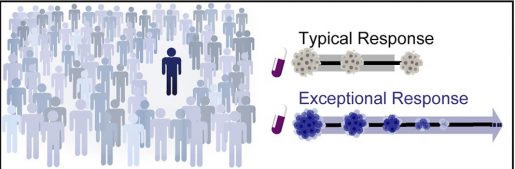
Exceptional responders are advanced-cancer patients who live much longer than other cancer patients with clinically comparable tumors. Looking to identify what helps exceptional responders defy the odds and the prognosis of dying of cancer, researchers at Baylor College of Medicine led a six-year study with the National Cancer Institute to analyze the tumor genome and microenvironment of exceptional responders to determine whether survival could be explained by genetic mechanisms.
“We wanted to know whether the genomes of exceptional responders could give us insights that could contribute to more effective therapy. The answer is yes, they can,” said Dr. David Wheeler, now a professor emeritus of molecular and human genetics at Baylor and lead author on the study. “Our analyses detected the Achilles’ heel — the genetic defects in these tumors that allow the cancer therapy to be more effective.”
Genomics points at cancer’s Achilles heel
The study examined 111 patients with different cancer types and treated with different therapies, all of whom displayed an exceptional response. Through genome sequencing analysis of the biopsied tumor, researchers were able to find genetic explanations for the exceptional response to therapeutics in about 25 percent of patients. Mechanisms contributing to therapeutic response fell into four categories — DNA-damage response, intracellular signaling, immune engagement, and genetic alterations characteristic of favorable prognosis.
For instance, the study revealed important insights about the cancer drug temozolomide, which works by damaging tumor DNA. The drug often is used to treat glioblastoma, an aggressive brain cancer with a short life expectancy of about 12 months. In typical glioblastoma cases, the tumor continuously repairs DNA damage caused by temozolomide, and soon becomes resistant, making the drug no longer effective. However, one exceptional responder from the study treated with temozolomide is tumor free 10 years after diagnosis.
We found that a key DNA repair pathway had been genetically inactivated in this patient’s tumor, so the tumor could not fix itself, making temozolomide lethal to the tumor,” said Wheeler, a member of the Dan L Duncan Comprehensive Cancer Center at Baylor.
“It turned out to be an Achilles’ heel for this tumor, revealing a critical role of this repair pathway in temozolomide treatment.”

Researchers also found the temozolomide-DNA-damage pathway to be important in exceptional responders with colon adenocarcinomas. In breast cancer patients, their analyses found that multiple mutations in the pathway that repairs DNA damage caused by platinum-based therapy to be a common theme.
“These findings are important because most current standard-of-care therapies involve DNA-damaging agents,” Wheeler said. “If you can identify the patients who have these DNA repair pathway mutations, oncologists may be able to predict who will benefit the most from these DNA-damaging cancer therapies. Then you might be able to lower the doses of these toxic agents and still have an effective treatment.”
In the case of a bladder cancer patient, researchers found the tumor’s immune microenvironment contributed to the patient’s exceptional response. The patient’s tumor was producing high levels of a protein usually produced by the immune system’s T cells. Patients with high amounts of the protein typically respond well to immune checkpoint inhibitor therapy. This small genetic mutation in the tumor made it vulnerable to immunotherapy, and as a result, the patient had a complete response and was still alive four years later with no tumor.
“This work demonstrates the importance of doing a genomic workup on every patient,” Wheeler said.
Every cancer patient is unique and requires a tailored therapy. You never know in advance who will be an exceptional responder, but a genomics approach may hold the key.”
Find all the details of this work in the journal Cancer Cell.
Baylor’s Human Genome Sequencing Center completed genome sequencing for this research, navigating the challenges of having only a small tumor biopsy sample available. Other contributors to this work from Baylor included Jianhong Hu, Donna M. Muzny, Harshavardhan Doddapaneni, and Viktoriya Korchina. See a full list of contributors and their affiliations, as well as financial contributions to this study in the full publication.
By Molly Chiu