Fighting back lymphoma resistance to treatment
T cell therapies have demonstrated encouraging results and benefits in patients with lymphoma resistant to chemotherapy, but, despite these advances, a large number of patients still respond poorly. A major advantage of T cell therapy is that it is highly targeted to tumor cells, so it does not cause bystander damage. Patients can have successful responses with virtually no toxicity, unlike their experience with chemotherapy and radiation.
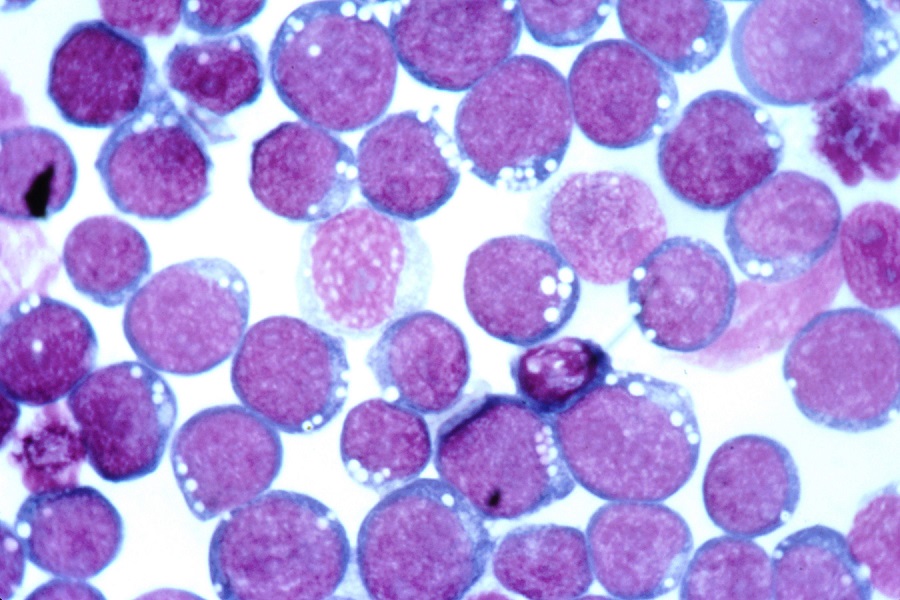
Like most tumors, lymphomas suppress immune responses engaged to destroy them. Tumors contain multiple cell types that secrete inhibitory molecules, including TGFβ. TGFβ inhibits the expansion and function of tumor-directed T cells, limiting their ability to eliminate tumors. To counter the tumor’s response against tumor-specific T cells, a team of researchers led by Dr. Cliona Rooney genetically modified these T cells so they cannot be affected by the inhibitory TGFβ signals of the tumor environment. They worked with T cells specifically directed at lymphoma caused by Epstein-Barr virus (EBV).

“We modified our EBV-specific T cells with a dominant-negative TGFβ receptor in which the intracellular signaling domain had been deleted. This mutant receptor can bind TGFβ but does not transmit an inhibitory signal and also blocks the inhibitory signaling of TGFβ through its normal receptor,” said Rooney, professor of pediatrics, division of hematology and oncology and the Center for Cell and Gene Therapy at Baylor College of Medicine, Texas Children’s Hospital and Houston Methodist Hospital.
The road to a first-of-its-kind clinical study
The research team began to investigate this strategy in 2002. Early studies showed that T cells expressing the dominant-negative TGFβ receptor could grow in the presence of TGFβ, while unmodified T cells failed to grow and died within two weeks. Later, they evaluated the strategy in animal models for safety and efficacy, which led to the design of the clinical trial.
“In an earlier clinical study of unmodified EBV-specific T cells (EBVSTs), more than 50 percent of patients experienced complete remission, and tumor responses were observed in over 70 percent,” said Rooney.
In the new study, patients who did not experience complete responses to unmodified EBVSTs had complete responses when they received T cells modified with the dominant negative TGFβ receptor.”
“These results come 18 years after this revolutionary approach was first conceptualized. While the study is small, its findings are encouraging for our patients’ families and for the cancer field,” said Dr. Catherine Bollard, now director of the Children’s Research Institute’s Center for Cancer & Immunology Research and previously at Baylor when the study was conducted, and first author of the study.
This research is a great illustration of bench-to-bedside work and the power of virus-specific T cells to produce significant patient response with little toxicity, the researchers said.
“After two bone marrow transplants and nearly two years of chemotherapy combined with weeks of radiation, my Hodgkin’s Lymphoma was still not in remission. The doctor who oversaw my transplants knew of the T cell trial at the Center for Cell and Gene Therapy and referred me for treatment. After speaking with Dr. Bollard and Vicky Torrano, it sounded like a worthwhile try since conventional treatment methods were not working,” said Nick Asoian, a participant in the trial who is based in Denver. “Over the course of about two years I had 12 infusions, and since my last infusion I have had many PET scans that are now showing no evidence of Hodgkin’s disease.”
Find all the details of this study in the Journal of Clinical Oncology.
###
Other contributors to this work include Conrad Russell Y. Cruz (formerly Baylor) and Cecilia Barese, Children’s National; Gianpietro Dotti (formerly Baylor), UNC; Stephen Gottschalk (formerly Baylor), St. Jude Children’s Research Hospital; Tamara Tripic, Olga Dakhova, George Carrum, Carlos Almeida Ramos, Hao Liu, Meng Fen Wu, Andrea N. Marcogliese, Adrian P. Gee, Malcolm K. Brenner and Helen E. Heslop, Baylor College of Medicine; Vicky Torrano, Youli Zu and Daniel Y. Lee, Houston Methodist; and Owen A. O’Connor, Columbia University Medical Center. The Baylor investigators are all members of the Dan L Duncan Comprehensive Cancer Center.
This work was supported by a National Institutes of Health SPORE in lymphoma and the Leukemia and Lymphoma Society.