CAR T cell therapy targeting HER2 antigen shows promise against advanced sarcoma in phase I clinical trial
Researchers at Texas Children’s Cancer Center and the Center for Cell and Gene Therapy at Baylor College of Medicine, Texas Children’s Hospital and Houston Methodist published results of a phase I clinical trial of a novel immunotherapy for high-risk sarcomas in the journal Nature Cancer.
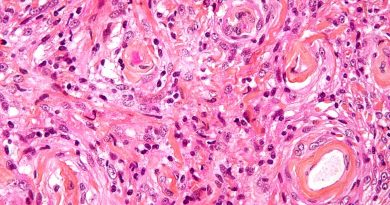
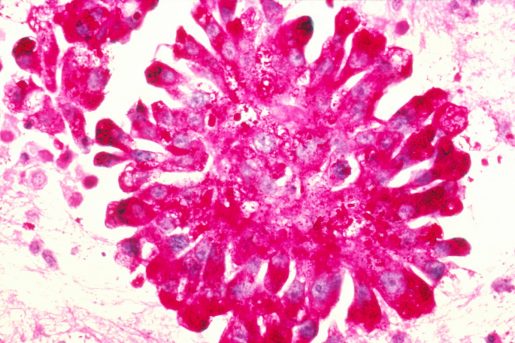
The therapy uses chimeric antigen receptor (CAR) T cells engineered to target the HER2 protein, which is overexpressed on the surface of sarcoma cells. Sarcoma is a type of solid cancer that develops in the bones and soft tissues. The HEROS 2.0 trial showed that this therapeutic approach is safe and is associated with clinical benefit.

“CAR T cell therapy has been a highly successful strategy for recurrent or high-risk leukemias or lymphomas, but challenges remain in using this therapy for solid tumors,” said first and corresponding author Dr. Meenakshi Hegde, associate professor of pediatrics – hematology and oncology at Baylor and pediatric oncologist at Texas Children’s Cancer Center. “The results of this trial show that we are moving the dial in harnessing the power of CAR T cells as an effective anticancer therapy for sarcomas.”
In a previous clinical trial, the HEROS study, researchers found that CAR T cells directed at HER2+ tumor cells had a favorable safety profile, but clinical benefit was limited by poor CAR T expansion and persistence. In HEROS 2.0, the second edition of the HEROS trials, researchers added successive HER2-CAR T cell infusions following lymphodepletion, which uses chemotherapy to deplete the patient’s own T cells, to make room for the infused therapeutic HER2-CAR T cells to expand.
“We also increased the number of allowable HER2-CAR T infusions to sustain the exposure time of CAR T cells, with the goal of increasing the antitumor effect,” Hegde said.
This study showed that CAR T expansion and persistence was improved with lymphodepletion and repeat cycles of treatment.”
Thirteen patients were enrolled in the HEROS 2.0 trial at Texas Children’s Cancer Center and Houston Methodist Hospital, and seven patients received multiple CAR T infusions. HER2-CAR T expansion occurred following 19 of 21 total infusions, and clinical benefit was seen in 50% of treated patients. An exceptional response in a patient with metastatic rhabdomyosarcoma was detailed in a publication in Nature Communications in 2020. The patient remains healthy and cancer free, more than five years after treatment.

Nine patients in the first two cohorts developed low-grade cytokine release syndrome (CRS), an acute inflammatory response seen as a side effect of CAR T treatment. Two patients in the third cohort experienced dose-limiting CRS, which necessitated ending the dose-escalation.
“We are now studying the tumors and the way we engineer the CAR T cells to better facilitate the safe delivery of higher doses, thereby enhancing antitumor activity by increasing the magnitude of CAR T cell expansion and persistence,” Hegde said.
“HEROS 2.0 exemplifies how the crosstalk between the bench and the bedside results in refinement of first-in-child studies and more durable clinical benefit,” said senior author Dr. Nabil Ahmed, professor of pediatrics – hematology and oncology at Baylor and pediatric oncologist at Texas Children’s Cancer Center.
The researchers currently are recruiting for the HEROS 3.0 trial, which will evaluate the safety of giving HER2-CAR T cells in combination with chemotherapy and an immune checkpoint inhibitor drug. Find more information on the trial here.
Hegde and Ahmed both are members of the Dan L Duncan Comprehensive Cancer Center at Baylor. Other study authors include Shoba Navai, Christopher DeRenzo, Sujith K. Joseph, Khaled Sanber, Mengfen Wu, Ahmed Z. Gad, Katherine A. Janeway, Matthew Campbell, Dolores Mullikin, Zeid Nawas, Catherine Robertson, Pretty R. Mathew, Huimin Zhang, Birju Mehta, Raksha R. Bhat, Angela Major, Ankita Shree, Claudia Gerken, Mamta Kalra, Rikhia Chakraborty, Sachin G. Thakar, Olga Dakhova, Vita S. Salsman, Bambi Grilley, Natalia Lapteva, Adrian Gee, Gianpietro Dotti, Riyue Bao, Ahmed Hamed Salem, Tao Wang, Malcolm K. Brenner, Helen E. Heslop, Winfried S. Wels, M. John Hicks and Stephen Gottschalk. They are affiliated with one or more of the following institutions: Baylor College of Medicine, Texas Children’s Cancer and Hematology Center, the Center for Cell and Gene Therapy, the Dan L Duncan Comprehensive Cancer Center, Dana Farber Cancer Institute, University of North Carolina at Chapel Hill, University of Pittsburgh, UPMC Hillman Cancer Center, Ain Shams University, Georg-Speyer-Haus Institute for Tumor Biology and Experimental Therapy, German Cancer Consortium, Frankfurt Cancer Institute and St. Jude Children’s Research Hospital.
This work was supported in part by Stand Up To Cancer (SU2C) – St. Baldrick’s Pediatric Cancer Dream Team Translational Research Grant (SU2C-AACR-DT1113), the V Foundation for Cancer Research, Triumph Over Kids Cancer Foundation (TOKC), Cookies for Kids’ CancerTM Foundation, Alex’s Lemonade Stand Pediatric Cancer Foundation, the Faris Foundation, National Cancer Institute and the Cancer Prevention and Research Institute of Texas. See the publication for a complete list of funding sources.
By Molly Chiu
Follow From the Labs on X @BCMFromtheLabs and Instagram!