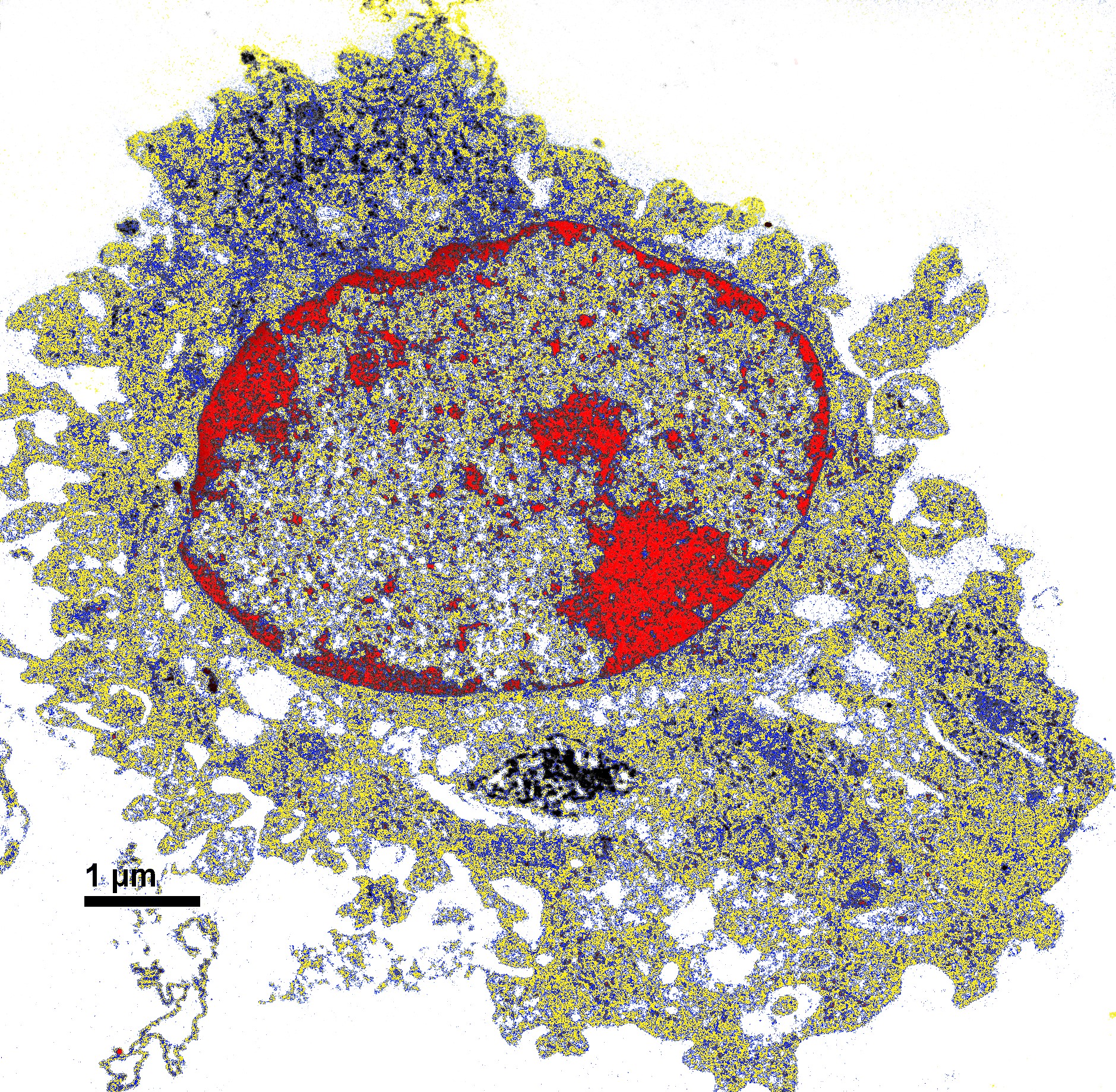
Unexpected viral behavior linked to type 1 diabetes in high-risk children
Viruses have long been suspected to be involved in the development of type 1 diabetes, an autoimmune disease, but consistent evidence connecting viruses to the condition has been hard to come by.
Investigators at the Baylor College of Medicine, the University of South Florida, and other institutions studied samples available through the TEDDY study, the largest prospective observational cohort study of newborns with increased genetic risk for type 1 diabetes, to address this knowledge gap. TEDDY studies young children in the U.S. (Colorado, Georgia/Florida and Washington State) and in Europe (Finland, Germany and Sweden).
“Type 1 diabetes occurs when the immune system destroys its own insulin-producing beta cells in the pancreas. Insulin is a hormone that regulates blood sugar in the body. Without it, the body cannot keep normal blood sugar levels causing serious medical complications,” said co-author Dr. Richard Lloyd, professor of molecular virology and microbiology and member of the Dan L Duncan Comprehensive Cancer Center at Baylor. “Type 1 diabetes is a life-threatening disease that requires life-long insulin injections to treat.”

“Years of research have shown that type 1 diabetes is complex and heterogeneous, meaning that more than one pathway that can lead to its onset,” said lead author Dr. Kendra Vehik, an epidemiologist and professor with University of South Florida’s Health Informatics Institute. “Type 1 diabetes is usually diagnosed in children, teens and young adults, but the autoimmunity that precedes it often begins very early in life.”

In the current paper, the researchers drew on the wealth of information available through the TEDDY study, which focuses on identifying environmental factors that can trigger type 1 diabetes in children who carry genes that increase their risk of getting the condition.
Unexpected viral behavior reveals new insights
Vehik, Lloyd and their colleagues studied the virome, that is, all the viruses in the body. They analyzed thousands of stool samples collected from hundreds of children followed from birth in the TEDDY study, looking to identify a connection between the viruses and the development of autoimmunity against insulin-producing beta cells.
Although Coxsackievirus, a type of enterovirus, has been implicated in type 1 diabetes before, the current results provide a completely new way to make the connection by identifying specific viruses shed in the stool. The investigators were surprised to find that it was a more prolonged infection of more than 30 days, rather than a short infection as was expected, that was associated with autoimmunity.
“This is important because enteroviruses are a very common type of virus, sometimes causing fever, sore throat, rash or nausea. A lot of children get them, but not everybody that gets the virus will get type 1 diabetes,” Vehik said. “Only a small subset of children who get enterovirus will go on to develop beta cell autoimmunity. Those whose infection lasts a month or longer will be at higher risk. A prolonged enterovirus infection might be an indicator that autoimmunity could develop.”
A new link between Coxsackievirus B and pancreatic beta cells
The researchers also discovered a new connection with Coxsackievirus B. Beta cells of the pancreas express cell surface proteins that help them talk to neighboring cells. One of these proteins also binds to the virus, acting as a receptor that allows it to attach to the cell surface of beta cells. The investigators discovered that children who carry a particular genetic variant in this virus receptor have a higher risk of developing beta cell autoimmunity.
This is the first time it has been shown that a variant in this virus receptor is tied to an increased risk for beta cell autoimmunity, a process that ultimately leads to the onset of type 1 diabetes,” Lloyd said.
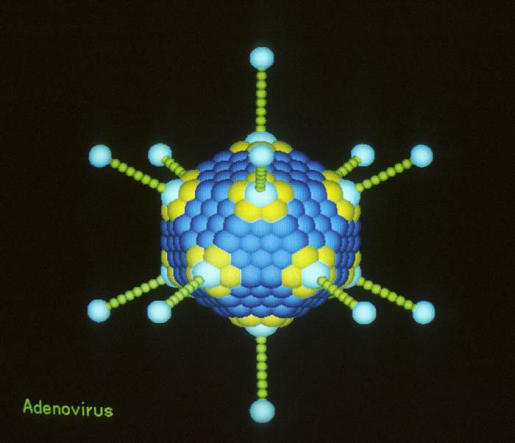
Another discovery was that the presence in early life of adenovirus C, a virus that can cause respiratory infections, was associated with a lower risk of developing autoimmunity. It remains to be investigated whether having adenovirus C in early life would protect from developing beta cell autoimmunity. Adenoviruses use the same beta cell surface receptor as Coxsackievirus B, which may offer one clue to explain this connection, although further research is needed to fully understand the details.
Other factors that affect autoimmunity and the development of type 1 diabetes are still unknown, but the TEDDY study is working to identify them. The researchers seek to gain insights into the exposures that trigger type 1 diabetes by studying samples that were taken before autoimmunity developed, starting when the TEDDY participants were 3 months of age. Such findings could identify approaches to potentially prevent or delay the disease.
“Taking it all together, our study provides a new understanding of the roles different viruses can play in the development of beta cell autoimmunity linked to type 1 diabetes, and suggests new avenues for intervention that could potentially prevent this disease in some children,” Vehik said.
Find all the details of this study in the journal Nature Medicine, including a list of all the authors, their affiliations and financial support for this study.
About TEDDY
The Environmental Determinants of Diabetes in the Young (TEDDY) study is a longitudinal, multinational study examining genetic-environmental causes of type 1 diabetes (T1D). The study follows children at high genetic risk for T1D from birth to 15 years of age at 6 clinical centers in the U.S. and Europe. TEDDY is funded by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), National Institute of Allergy and Infectious Diseases (NIAID), Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), National Institute of Environmental Health Sciences (NIEHS), Centers for Disease Control and Prevention (CDC), and JDRF. More information can be found on the TEDDY study website.