Together, DAG1 and Yap ‘hit the brakes’ on heart cell proliferation
Although both are known to play a role in cardiac function and previous work had hinted that they might interact with each other, it was not clear that the dystrophin glycoprotein complex (DGC) pathway and the Hippo pathway worked together to affect heart cell proliferation. The James Martin lab at Baylor College of Medicine explored this possibility and their findings have implications for both heart regeneration after injury and also for improving cardiac function in children with muscular dystrophy.
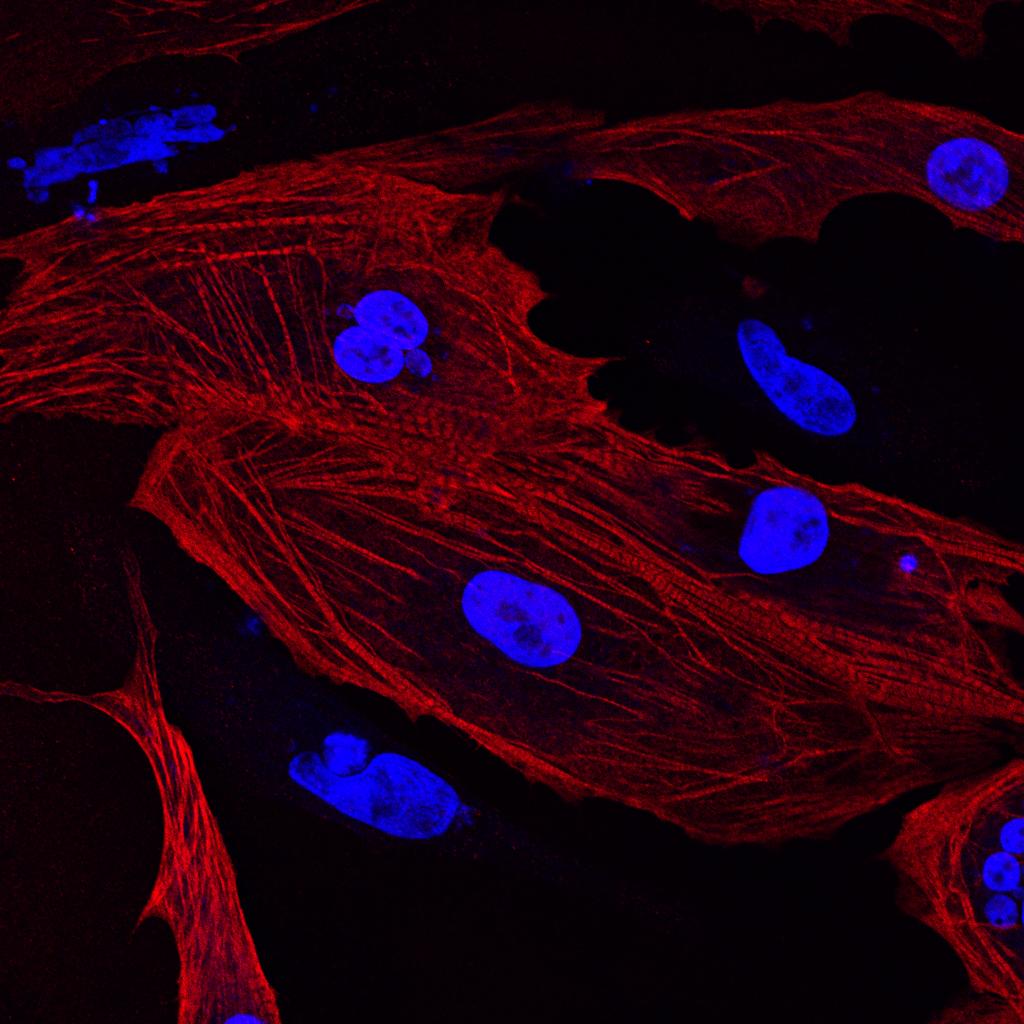
“We are investigating the question of why the heart muscle doesn’t renew,” said Dr. James Martin, professor and Vivian L. Smith Chair in Regenerative Medicine at Baylor College of Medicine and Director of the Cardiomyocyte Renewal Lab at the Texas Heart Institute. “In this study, we focused on two pathways of cardiomyocytes or heart cells: the Hippo pathway, which is involved in stopping renewal of adult cardiomyocytes, and the DGC pathway, which is essential for cardiomyocyte normal functions. We are also interested in studying mutations in DGC components because patients with these mutations have a muscle wasting disease called muscular dystrophy.”

The heart muscle is one of the least renewable tissues in the body, which is one of the reasons that heart disease is the leading cause of death for both men and women in the United States, according to the Centers for Disease Control and Prevention.
When DAG1 captures Yap….
In this study, Martin and colleagues studied the consequences of the interaction between components of the DGC pathway with members of the Hippo pathway in animal models. The researchers genetically engineered mice to lack genes involved in one or both pathways, and then determined the ability of the heart to repair an injury. The results showed for the first time that dystroglycan 1 (DAG 1), a component of the DGC pathway, directly binds to Yap, part of the Hippo pathway, and that this interaction inhibited cardiomyocyte proliferation.
The discovery that the Hippo and the DGC pathways connect in the cardiomyocyte and that together they act as ‘brakes,’ or stop signals to cell proliferation, opens the possibility that by disrupting this interaction one day it might be possible to help adult cardiomyocytes proliferate and heal injuries caused by a heart attack, for example,” Martin said.
Another long-term application of this discovery could be to improve cardiac function in children with muscular dystrophy.
“Patients with muscular dystrophy can have severe reduction in cardiac function,” Martin said. “Our findings may help to design medicines to slow down cardiac decline in muscular dystrophy by stimulating cardiomyocyte proliferation. In order to do that, we need more research to understand cardiomyocyte growth control pathways in greater detail.”
Read the complete report in Nature.
###
Other contributors to this work include Yuka Morikawa, Todd Heallen, John Leach and Yang Xiao.
This project was supported in part by an Intellectual and Developmental Disability Research Center grant (1U54 HD083092) from the Eunice Kennedy Shriver National Institute of Child Health and Human Development; the Mouse Phenotyping Core at Baylor College of Medicine with funding from the National Institutes of Health (U54 HG006348); and grants from the National Institutes of Health (DE 023177, HL 127717, HL 130804, and HL 118761) and the Vivian L. Smith Foundation. Support was also provided by the Transatlantic Network of Excellence Award LeDucq Foundation Transatlantic Networks of Excellence in Cardiovascular Research 14CVD01 and the American Heart Association Scientist Development Grant 16SDG26460001.