Q&A: What you should know about VATS lobectomy

Early stage lung cancer patients may have a less invasive option when it comes to surgery.
Baylor College of Medicine Thoracic Surgeon Dr. Bryan Burt says video-assisted lobectomies are becoming a more common technique for treating select patients.
Burt, an assistant professor in the Michael E. DeBakey Department of Surgery, who specializes in thoracic surgical oncology, explains what a lobectomy is and what you need to know about it in the following Q&A.
Q: What is a lobectomy?
A: A lobectomy is an operation to remove a portion, or lobe, of the lung. This surgical procedure is commonly performed for patients with lung cancer.
A lobectomy can be performed in two ways:
-
Through an incision on the chest, called a thoracotomy. This is the traditional way to perform a lobectomy. This procedure is often also referred to as “open” lobectomy.
- Through a minimally invasive procedure, called Video Assisted Thoracic Surgery or VATS lobectomy. This procedure is also referred to as thoracoscopic lobectomy
Q: Which patients are candidates for this procedure?
A: Patients with early stage lung cancer are candidates for these procedures. Certain patients with other cancers that have spread to the lungs are also occasionally candidates for this procedure.
Q: What are the benefits of VATS lobectomy versus traditional lobectomy?
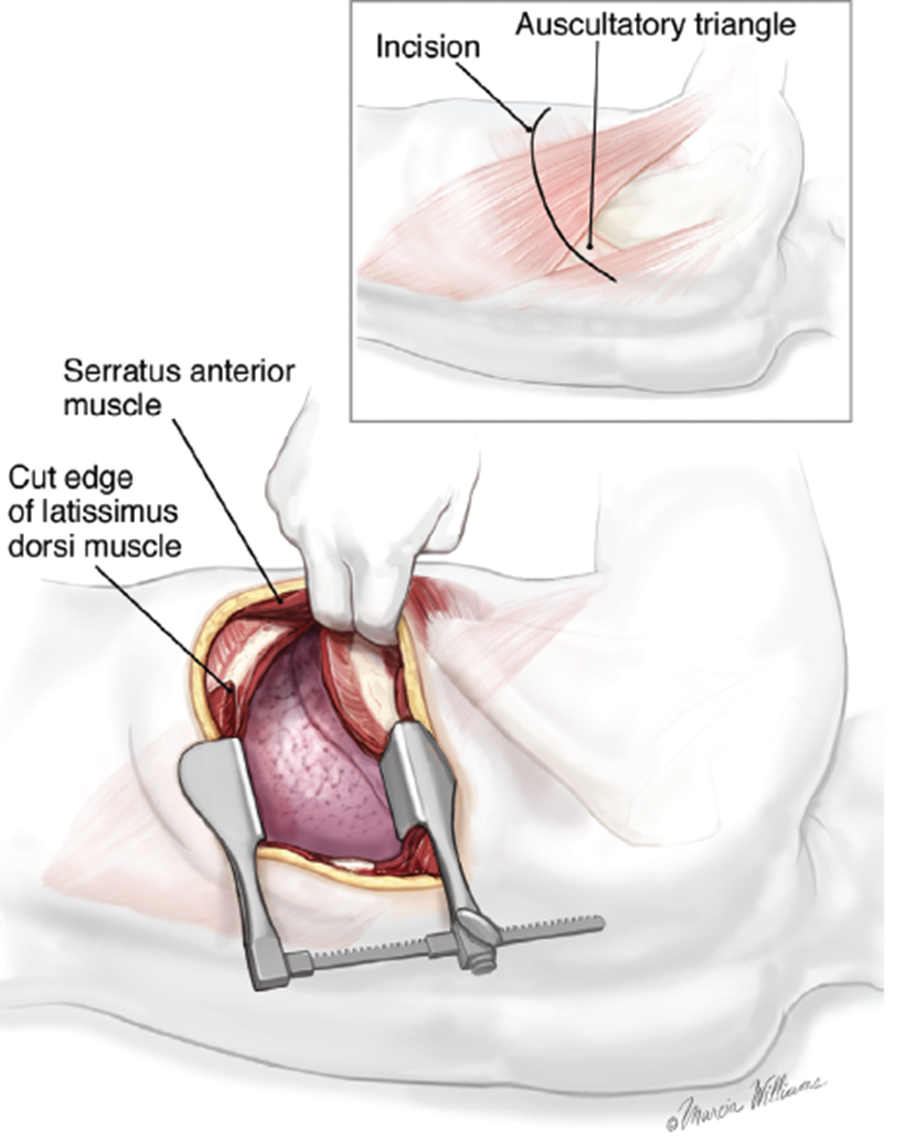
A: Traditional lobectomy (open lobectomy) is performed through a thoracotomy, which is a relatively large incision in the chest.
On the other hand, VATS lobectomy can be performed through three small incisions.
This approach to lobectomy can be completed safely and has several benefits that an open lobectomy does not offer:
- An overall faster recovery and return to work
- Decreased pain
- Decreased postoperative complications
- Decreased length of chest tube drainage after the procedure
- Decreased hospital stay (patients typically go home in 2-3 days)
- Improved quality of life
- Smaller surgical scars
Q: What happens during VATS lobectomy?
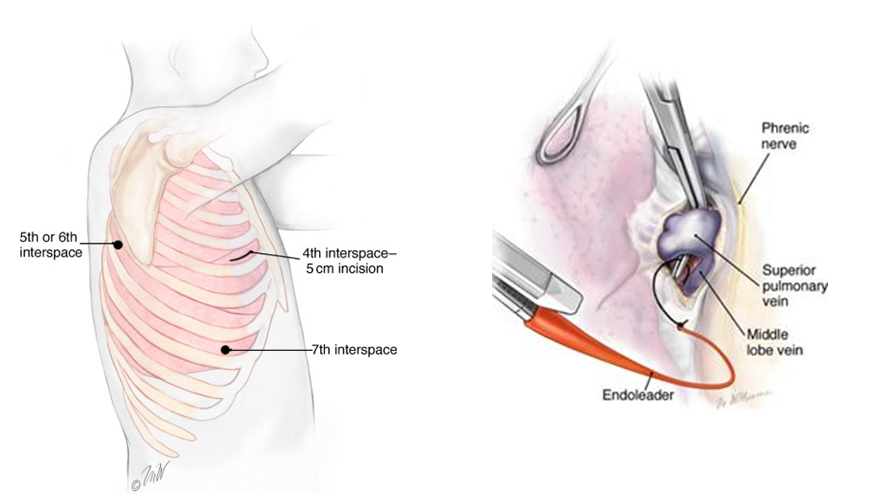
A: During VATS lobectomy, the surgeon makes three small incisions on one side of the patient and inserts a thin tube-like instrument, called a thorascope, through one of the incisions.
The thorascope has a tiny camera on one end that allows the surgeon to see the lungs on a video monitor.
The surgeon uses the other two incisions to place working instruments. In this way, the surgeon is able to perform the work necessary to remove the portion of the lung (the lobe) that contains the cancer.
Lymph nodes are also removed from the chest to test whether the cancer has spread to these sites.
When the operation is finished, the surgeon will temporarily place one tube in the chest to drain fluid and air, and close the incisions.
Q: How common is VATS lobectomy for the treatment of lung cancer?
A: The use of VATS lobectomy has increased in the last 10 years, particularly in specialty centers such as Baylor St. Luke’s Medical Center. As patients become more aware of the efficacy and safety of the procedure, it is becoming more common to treat early stage lung cancer using this technique.
Q: How many VATS lobectomies do you do each year?
A: I typically perform 40-50 of these procedures each year.
Q: What tests do you perform to evaluate whether a patient is a candidate for the procedure?
A: To determine whether a patient is a candidate for this procedure, I typically obtain a chest computed tomography scan. CT is a procedure that uses special X-ray equipment to create images of organs inside the body. I also do tests to evaluate pulmonary function, including a positron emission tomography-CT scan. PET-CT scans of the lungs provide information about both the function and the structure of the organ in a single session.
If you are thinking of treatments for early stage lung cancer, consider consulting with a thoracic surgical oncologist about VATS lobectomy. To schedule a consultation with Dr. Burt, call (713) 798-6376.
Learn more about VATS lobectomy.
For more information about this and other diagnostic and treatment services for cancer and other disorders of the lung, esophagus, mediastinum, and chest wall, visit the Lung Institute.
–By Ana María Rodríguez, PhD; Sr. Medical Editor, Michael E. DeBakey Department of Surgery