CAR T cell therapy makes strides in tackling Hodgkin lymphoma
Most patients with Hodgkin lymphoma (HL), a type of cancer of immune cells called B lymphocytes, are cured with first-line therapy, but approximately 15 percent have primary refractory disease or relapse after an initial response to treatment.
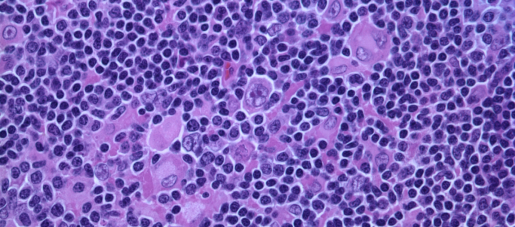
Dr. Carlos Ramos at Baylor College of Medicine and his colleagues at Baylor and the University of North Carolina Lineberger Comprehensive Cancer Center have tackled relapsing or refractory HL with a novel treatment combination that produced promising results in a clinical trial.
“In a 2017 pilot study in seven refractory/relapsing Hodgkin lymphoma patients, Baylor and UNC researchers found that a CAR-T cell therapy targeting Hodgkin cell-associated protein CD30 appeared safe but brought about only modest responses,” said Ramos, co-first author of the study and professor in the Margaret M. and Albert B. Alkek Department of Medicine and the Center for Cell and Gene Therapy at Baylor, Houston Methodist Hospital and Texas Children’s Hospital.

In the new study, which included 41 patients treated at Baylor and UNC, the researchers used the same anti-CD30 CAR-T cell strategy, but added a preparative regimen in which patients’ existing lymphocytes – a broad family of white blood cells including T cells – were greatly depleted with chemotherapy drugs prior to the addition of the CAR-T cells.
A promising combination
The combination of lymphodepletion with anti-CD30 CAR-T led to the complete disappearance of tumor in the majority of patients treated at the highest dose level of therapy, with almost all patients having clinical benefit after treatment,” said Ramos, a member of the Dan L Duncan Comprehensive Cancer Center at Baylor.

“Lymphodepletion prior to CAR-T cell infusion seems to produce a more favorable environment for the CAR-T cells to proliferate and attack their cancerous targets,” said Dr. Natalie Grover, study co-first author, assistant professor in the UNC Department of Medicine and a UNC Lineberger member.

“These results are particularly exciting because the majority of these patients had lymphomas that had not responded well to other powerful new therapies,” said study senior author Dr. Barbara Savoldo, professor in the UNC Department of Microbiology and Immunology at the UNC School of Medicine and a UNC Lineberger member. “Everyone worked tirelessly on the study, and I am proud of the collaborative work it fueled between UNC Lineberger and Baylor.”
“I am very pleased to see this strategy, developed by Dr. Savoldo when she was at Baylor and initially translated to the clinic with Dr. Ramos, has now been validated in larger clinical trials at two centers,” said co-author Dr. Helen Heslop, director of the Center for Cell and Gene Therapy and a Dan L Duncan Chair at Baylor.

Side effects of the lymphodepletion plus CAR-T cell treatment were common and included flu-like symptoms due to an immune chemical storm called cytokine release syndrome, but these events were generally modest. None of the patients experienced the more serious, life-threatening complications, such as brain swelling, that have been seen in CAR-T cell trials against other blood cancers.
As the trial progressed, the researchers settled on fludarabine as a key element of the pre-therapy lymphodepletion regimen, since patient outcomes seemed better when it was used. The researchers found that among the 32 patients with active cancer who received fludarabine for lymphodepletion before their CAR-T cells, 19 patients (59 percent) had a complete response.
Of the patients in the study who had a complete response, 61 percent still had no evidence of recurrence a year later. Overall, 94 percent of the treated patients were still alive a year after their treatment.
One patient’s remarkable recovery is detailed in the Dan L Duncan Comprehensive Cancer Center Annual Report. The researchers hope to do further studies of the CAR-T cell therapy alone and in combination with other new immune-modulating anticancer drugs.
Read the complete study in the Journal of Clinical Oncology
Other authors who contributed to this work include Dr. Anne W. Beaven, Dr. Premal D. Lulla, Meng-Fen Wu, Dr. Anastasia Ivanova, Dr. Tao Wang, Dr. Thomas C. Shea, Dr. Cliona M. Rooney, Christopher Dittus, Steven I. Park, Dr. Adrian P. Gee, Dr. Paul W. Eldridge, Kathryn L. McKay, Birju Mehta, Catherine J. Cheng, Faith B. Buchanan, Bambi J. Grilley, Dr. Kaitlin Morrison, Dr. Malcolm K. Brenner, Dr. Jonathan S. Serody and Dr. Gianpietro Dotti. The authors are affiliated with Baylor College of Medicine and the University of North Carolina at Chapel Hill.
The research was supported by the National Institutes of Health (RO1HL114564, P50CA126752, P30 CA125123, K12CA120780), the University Cancer Research Fund, and the Leukemia Lymphoma Society.
By Molly Chiu