Comfort care or medical treatment?
Before former first lady Barbara Bush passed away on April 17, 2018, it was widely reported that she had “decided not to seek additional medical treatment and [would] instead focus on comfort care.” This announcement generated renewed discussion about palliative care in the news and on social media.
On one hand, palliative care specialists commended Mrs. Bush, who was known to have chronic obstructive pulmonary disease and congestive heart failure, for making her decision public.
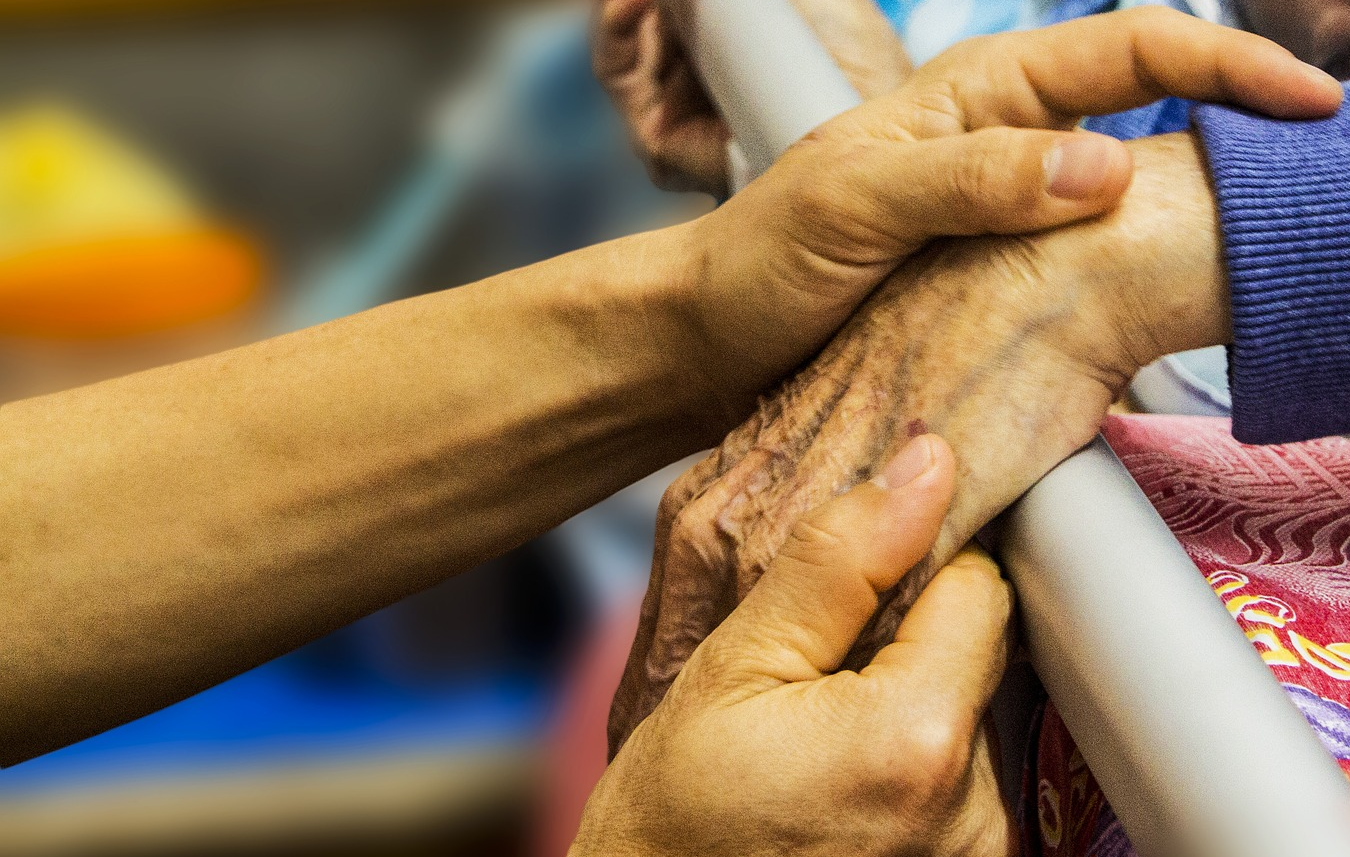 On the other hand, there was consternation that the decision was presented as “comfort care” vs. “medical treatment.” Many chastised the news media for furthering a false dichotomy, until it became clear that the language in fact came from the family’s statement.
On the other hand, there was consternation that the decision was presented as “comfort care” vs. “medical treatment.” Many chastised the news media for furthering a false dichotomy, until it became clear that the language in fact came from the family’s statement.
The consternation is understandable. Palliative care, both as a concept and as a medical specialty, still contends with the longstanding American cultural value that disease and death are enemies to be battled, and that any choice to forgo available medical interventions means “giving up.”
Indeed, Mrs. Bush’s granddaughter, Jenna Bush Hager, told the Today Show after the announcement, “She’s in great spirits and she’s a fighter.” This description of a loved one as “a fighter” is familiar to everyone who has helped families make difficult decisions about care near the end of life.
To counter the notion that declining further attempts at life-prolonging interventions represents a moral failure on the patient’s part, providers often frame palliative care as simply a different form of aggressive medical care.
In this frame, the goals of care may have shifted, but the medical team is still delivering advanced treatment to control symptoms and maximize quality of life. I’ve had these conversations many times with patients in my role as an oncologist and palliative care doctor.
Thus, when I first read the words “decided not to seek additional medical treatment,” I shared my colleagues’ frustration that comfort care was not viewed as medical treatment.
Then I reconsidered. After all, the statement came from the family; whatever I think about palliative care, this was how they chose to describe it. Perhaps, rather than regard their description as an unfortunate choice of words, we should listen to the words.
We feel that we’ve failed, or are devalued as a specialty, when patients view comfort care as something other than medical treatment. But maybe what they’re trying to tell us is that they see a difference between a highly technological, medicalized death and a more natural drawing to a close. In that case, we are there with them not to make a diagnosis or cure a disease, but for one deeply humanistic purpose: to ease suffering.
If a patient and her family call this kind of care something other than medical treatment, maybe we should listen. In the end, it’s their story, not ours.
-By Dr. Stacey Berg, professor of pediatrics-hematology and oncology at Baylor College of Medicine