New insights from an autoimmunity-mediated atherosclerosis mouse model could pave the way to new therapies for cardiovascular diseases
By Ana María Rodríguez, Ph.D.
Patients with autoimmune disease have a higher risk of developing atherosclerosis and cardiovascular disease. Although studies have shown that human atherosclerotic plaques typically have antibodies against self-antigens, the role those complexes or immune cells play in the development of atherosclerotic lesions is still under investigation. To study how autoimmunity may lead to atherosclerosis, researchers from Baylor College of Medicine, INSERM, and the University of Bordeaux have developed a mouse model and used a well-adapted experimental proteomic approach to identify specific aortic self-antigens targeted by the animal’s immune system and involved in the development of atherosclerosis. Their results appear in the June issue of FASEB Journal.

“In our mouse model we show that the extent of autoimmune responses, the identification of their specific targets and the distribution of the latter in the vascular wall highlight an underestimated role of autoimmunity in cardiovascular diseases. Our results place autoimmunity in the driver’s seat in the engine of atherogenesis and propose novel mechanisms for the buildup of lesions,” said corresponding author Dr. Aksam Merched, assistant professor of molecular and cellular biology at Baylor and currently at the University of Bordeaux.
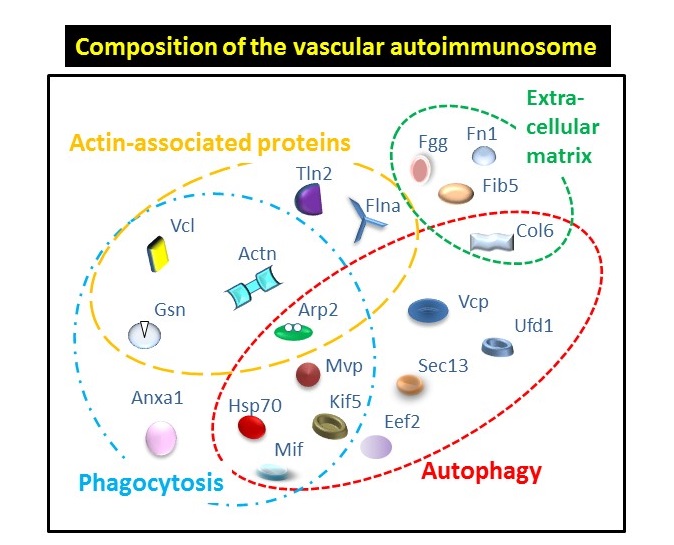
The researchers created a model that amplified the autoimmune responses in order to detect their targets in the blood vessels and study the progression of atherosclerosis. Using this model, they determined that the mouse’s immune system produced an immune response toward 19 different proteins located on the vascular wall. Most of these proteins belong inside the cell and are released and detected by the immune system after cells are damaged. “We propose that the antibodies against self-proteins bind to them, triggering further immune mechanisms that may contribute to the amplification of damage to the vasculature, providing a foundation for the build-up of atherosclerotic lesions,” said Merched.
“By identifying potential targets for the autoimmune response, this study may help in the development of new biomarkers, such as specific autoantibodies, which may be used in diagnostic applications or to monitor the efficacy of therapeutic interventions,” said Merched.
At the same time, these findings provide a rationale for the use of therapies to suppress the response against these self-antigens. The creation of immune tolerance vis-à-vis these autoantigens may open up a new therapeutic avenue in cardiovascular diseases.
The following authors also contributed to this work: Danièle Daret, Lan Li, Nathalie Franzl, and Maria Sauvage-Merched, from INSERM and the University of Bordeaux, France.
This work received grant support from the American Heart Association (SDG 0730172N) and Marie Curie Actions (FP7 Intra-European Fellowship PIEF-GA-2009-237028).