Using artificial intelligence to advance healthcare globally
It may be surprising to learn that artificial intelligence (AI) is as old as the computer. Although its origins date back to the 1940s and 1950s, no other concept evokes as much fear as AI, but its ability to assist with medical treatment generates hope.
For over a decade, Baylor Global Health and Rice University’s Department of Bioengineering has researched how to use AI for gastrointestinal (GI) cancer screening. They are finding ways to use microendoscopy technology for cancer screening by reducing the cost of it and making platforms that are small and battery-operated.
“We want to reduce the barrier to undergoing endoscopy and have a lasting impact on endoscopic cancer screening and prevention,” said Dr. Sharmila Anandasabapathy, professor of medicine, gastroenterology and vice president of Baylor Global Health. “The microendoscopy technology is something that the field of GI has used for almost two decades now, but current platforms are expensive and require a lot of user expertise.”
The collaboration has led to clinical trials in China, Honduras and throughout the United States.
“The computer will provide a diagnosis of the tissue—cancer, pre-cancer or benign—in real-time, but the doctors’ eyes are also on the tissue,” Anandasabapathy said. “What we want to find out in this study is whether the computer diagnosis is comparable to the expert doctors, whether the expert doctors’ confidence is improved by the computer diagnosis and whether new, young doctors in training are more accurate when the computer is providing the diagnosis. Our end goal is to make GI cancer prevention more accessible, affordable and impactful.”
AI is the use of complex computer algorithms to solve human problems without the direct involvement of humans. These complex computer algorithms exhibit behaviors that resemble human intelligence, somewhat like an electronic brain. AI enables computers to perform human tasks at a level that are either equally as good or more advanced than its human counterpart.
This technology offers well-defined end-user output through machine learning (ML) algorithms, which build a mathematical model from sample training data, recognize patterns, make predictions and form conclusions on their own to perform useful tasks.
The growing field of artificial intelligence in medicine (AIM) involves healthcare-related AI applications that diagnose disease, suggest diagnostic and therapeutic recommendations, and analyze relationships between either preventive care, diagnosis or treatment and patient outcomes. AI in healthcare offers the dual advantage of lowering healthcare costs and improving the accuracy of diagnosis and treatment measures.
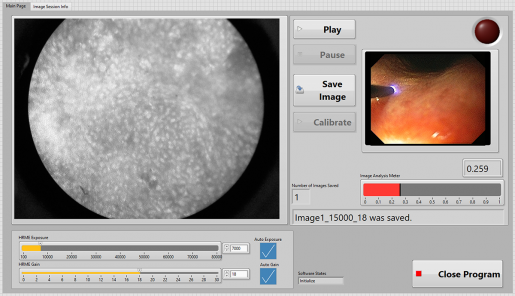
The Brazil High-Resolution Microendoscopy (HRME) is one of the trials that hopes to leverage all the benefits of AI, including its efficiency, low cost and ability to reduce workload and relieve workforce capacity to decrease the prevalence of deadly gastrointestinal cancers like esophageal cancer. Esophageal cancer is the sixth-leading cause of cancer mortality in the world, accounting for more than 500,000 global cancer deaths each year. Brazil, and most of Latin America, has severe capacity limitations, such as equipment, infrastructure and clinicians, which prevent the early detection of esophageal cancer.
“In Brazil and Latin America, squamous cell cancer of the esophagus and gastric adenocarcinoma are still prevalent diseases,” said Dr. Fauze Maluf-Filho, director of the endoscopy unit at Instituto do Câncer do Estado de São Paulo (ICESP). “I think that if you have artificial intelligence with a high-resolution microendoscopy device available, it will improve the way that we perform cancer screening in our region.”
The purpose of AI technology is to solve problems, not create fear. One part of this trial investigates the device’s acceptability among patients, healthcare providers, health systems, healthcare leaders and administrators and identifies any barriers to implementation in a real-world environment.
“Upon review of the preliminary data, people are really excited about the potential for HRME and computer-assisted diagnosis in addressing patient barriers, minimizing the burden on patients and making healthcare more equitable,” said Dr. Jane Montealegre, deputy director of the office of outreach and health disparities at the Dan L Duncan Comprehensive Cancer Center (DLDCCC) and assistant professor in pediatrics at Baylor.
-By Brodus Franklin, M.D., MHA, MBA, business operations associate, Baylor Global Health



