How immunotherapy is transforming cancer treatment and patient care
From surgical intervention to targeted therapies, a wide range of treatment options are now available for many patients with cancer. Immunotherapy is a tool that physicians and researchers in the Dan L Duncan Comprehensive Cancer Center at Baylor College of Medicine are using to advance new cancer treatments options.
But what is immunotherapy?
Dr. Andrew Sikora, vice chair of research in the Department of Otolaryngology and co-director of the head and neck cancer program at Baylor, breaks down exactly what immunotherapy does to the body to treat cancer.
Q: How does immunotherapy work?
A: Your immune system’s main job is to defend your body against invaders, like infectious organisms or cancer cells. However, cancer cells often pass through the immune system’s defense because they look so similar to healthy tissue.
Immunotherapy is the act of retraining your immune system’s defense system so it can identify and fight cancer cells.
Currently there are several ways in which immunotherapy is administered to patients, including:
- Cancer vaccines: Preventative cancer vaccines, such as the HPV vaccines Cervarix and Gardasil, can prevent cancers from developing. For patients who have developed cancer, therapeutic vaccines are designed to stimulate the body’s own immune response against the tumor. An FDA-approved therapeutic cancer vaccine exists for prostate cancer, and vaccines are currently in clinical trials for many other tumor types.
- Checkpoint inhibitors: Checkpoints are molecules on the surface of white blood cells that prevent excessive immune responses from attacking your body. However, cancer cells have created ways to use these checkpoints to shut down the immune system.Checkpoint inhibitors are drugs that target your body’s checkpoints. They block the checkpoint molecules or the molecules on tumor cells which activate them, and thus allow the immune system to become active against cancer cells. Checkpoint inhibitors are FDA-approved for melanoma, lung cancer, head and neck cancer, and renal cell carcinoma.
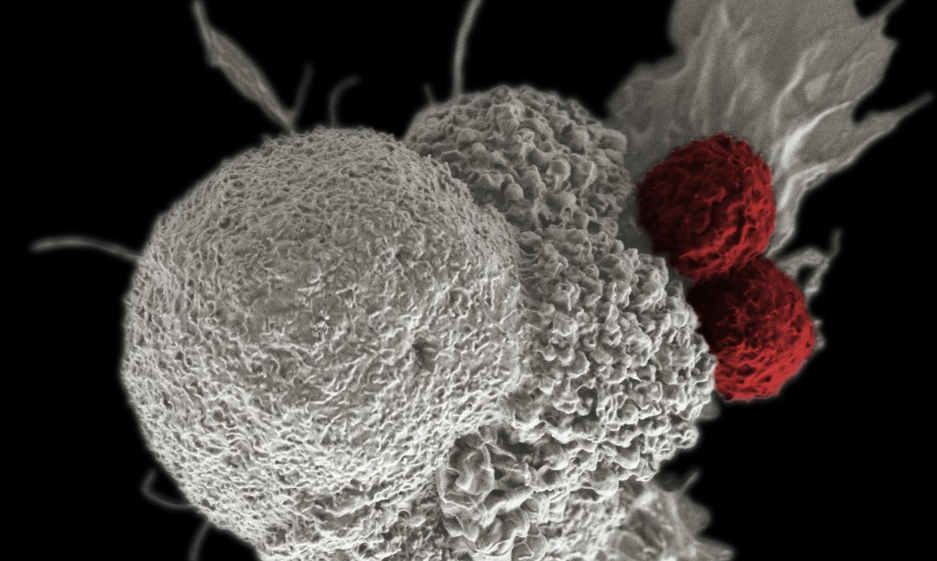
- Adoptive T cell therapy: T cells are white blood cells that protect you from illness and disease. T cell therapy consists of isolating your own T cells (from blood or tumor samples), and manipulating the cells in a lab, training them to fight your particular cancer cells. The T cells are then reinfused into you intravenously.The goal of T cell therapy is usually to make your own T cells more active and thus more effective at identifying and killing tumor cells. Adoptive T cell therapy is approved for melanoma and certain leukemias and lymphomas, and in clinical trials for many other tumor types. The Department of Cell and Gene Therapy at Baylor College of Medicine is one of the world’s leading research groups for this type of immunotherapy.
- Antibody-based therapy: Antibodies are a type of protein produced by your body that identifies and neutralizes bacteria and viruses. Antibodies specific for molecules which appear on cancer cells can be used to treat many different tumor types. In treatment, the antibodies are delivered intravenously into your body either on their own or attached to chemotherapy drugs or radioactive particles.
- Oncolytic virotherapy: Oncolytic virotherapy uses viruses that selectively kill tumor cells, usually by injection directly into the tumor. In addition to directly killing tumors, oncolytic viruses induce a powerful immune response. Oncolytic viruses are approved for melanoma, glioma, ovarian and certain pancreatic cancers.
Q: Can immunotherapy be used with other cancer treatments?
A: Combination treatments are being developed that test immunotherapy in combination with conventional treatments such as chemotherapy and radiation.
Q: Why is immunotherapy important to advancing cancer therapy overall?
A: All immunotherapies ultimately rely on activating the patient’s own immune system. The immune system is capable of changing over time and “learning” how to better target cancer cells, and therefore is capable of keeping up with the cancer cells, which often escape other treatment methods by mutating.
Once activated, the patient’s immune system can patrol the body and prevent cancers from recurring. These theoretical advantages of immunotherapy have been proven effective in an increasing number of clinical trials for diverse cancer types.
Additional Resources
Read more about immunotherapy care for head and neck cancer.
Visit the National Cancer Institute website for more information about immunotherapy.
-By Eliana Amram



